Did you know that depending on the source, there are either 1 in r or 1 in 5 women with a retroverted uterus, also known as a tipped uterus, retroflex uterus or tilted uterus?
Health is the most important aspect of our lives and our greatest goal – or at least it should be. Every woman tries to take care of her body, and in the perspective of a pregnancy, the health of the reproductive system is essential. A retroverted uterus during pregnancy is a very serious issue that concern many women.
Table of Contents
What Is a Retroverted Uterus?
The uterus is a cavity with a shape of overturned pear. The average length is of 6 to 8 cm, and the average length is of 3 – 4 cm. Its walls are externally formed from thin muscle tissue, while inside is lined with a mucosa known as endometrium. This mucosa, designed to host the fertilized egg, rich in gnadular structures and blood vessels, undergoes essential changes depending on the woman`s age or menstrual cycle periods, under the hormonal influence. – Visit us here!
The lower part of the uterus, the narrowed region of the vagina, is known as the cervix. During pregnancy, the uterus`s size increases quite a lot – its height is of around 30 cm at the end of pregnancy.
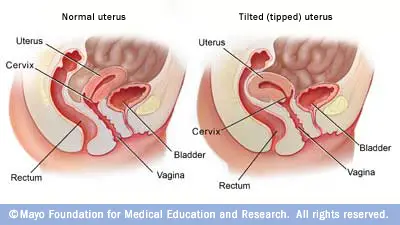
So, what does it mean to have a tilted uterus? A retroverted uterus represents a uterus which is tilted posteriorly (tilted backwards towards the spine). The woman`s vagina isn`t positioned vertically inside the pelvis; it`s inclined towards the lower back. This represents the contrast of the “anteverted” uterus which most women have (this type of uterus is tilted forward toward the woman`s bladder.
While the retroverted uterus doesn`t cause problems in most cases, some women feel various signs, including pain during sexual intercourse.
Normal Position of the Uterus
The uterus is positioned next to the vagina, in a slightly inclined position towards the front, above the bladder. This specific position is known as “anteversion” and is considered the normal position of a woman`s uterus. The uterus is supported by ligaments which give it some sort of flexibility and at the very same time prevents it from descending into the vagina.
The uterus might change its position slightly during the menstrual cycle. Sometimes it might happen that the uterus`s position is also a bit oriented “backwards”. This particular position is known as “retroverted.” In this particular case, we talk about a retroverted uterus. Sometimes, the uterus`s position can also be inclined towards the right or left.
Causes
In most cases, retroverted uterus is congenital, but there might be other factors that lead to a change of its position in time. Here are a few important ones:
- Pregnancy – Another natural cause which can make as a normal uterus to become retroverted is pregnancy. After birth, the ligaments supporting the uterus lose their elasticity and tonicity, and the uterus instead of returning to the normal position (forward), it “falls” in the retroverted position (backwards).
- Endometriosis – Endometriosis might cause the uterus to be “pulled” and “held” in the retroverted position by endometrial tissue outside the uterus. Due to this reason, the uterine mobility may suffer, being “forced” to stand in a position that isn`t normal.
- Adhesions – An adherence represents a scar tissue which clutches 2 different anatomical surfaces (in general). Pelvic surgical interventions may lead to adhesions which may pull the uterus in a tilted position.
- Fibroids – These are quite small (non-cancerous), but might make the uterus sensitive to tilt on the back.
- Sexual Issues – In most cases, the ovaries and fallopian tubes are tipped backwards. This means that all these structures can be pushed out during a sexual contact, which is known as dysentery. If sexual contact is strong, the ligaments around the uterus might be injured or broken.
Signs & Symptoms
There are a series of different symptoms that were associated with a retroverted uterus. Still, there lots of cases in which the woman show no symptom. The main signs are:
- Pain during sexual contact or
- Pain during menstruation or dysmenorrhea.
- Minor incntinence.
- Urinary tract infection.
- Fertility issues.
- Difficulties in using the tampons.
Analyzes & Diagnosis
Na laborious investigations are needed to diagnose a retroverted uterus. A transvaginal ultrasound is quite efficient for this particular medical condition. – Read this!
Diagnosis is done at a simple pelvic exam, the gynecologist being able to determine the position of the uterus quite easily. Also, the diagnosis of a retroverted uterus can also be made by ultrasound.
Retroverted Uterus during Pregnancy
In most cases, a retroverted uterus isn`t considered a cause of infertility, although if all other possible complication were excluded, an expert in fertility might recommend surgery to rectify the position of the uterus.
The ability of sperm to reach the uterus has nothing to do with its position. Having a retroverted uterus can be a normal anatomical variation, just like the color of the eyes or hair. – Read more!
Still, such a uterus may affect fertility in some way, because sperm may get a little harder in the uterus, but this may be influenced by choosing certain sexual positions during or after intercourse (e. g. the woman lying on her stomach).
Secondly, if the adhesions formed in the pelvic area have a retroverted uterus, they hinder the movement and flexibility of the uterus and fallopian tubes, and this may lead to the occurrence of difficulties in conception.
Starting with the weeks 10 – 12 of pregnancy, your uterus will no longer be tilted, and only in rare cases this doesn`t move in the middle position. In case this happens, then it`s possible for a miscarriage to occur. However, this rarely happens.
Treatment
Possible therapies for retroverted uterus with incarceration include the following:
- Bladder decompression by catheter drainage.
- The adoption of special position: knees to the chest, sleeping in the pronated position.
- Manual uterine repositioning with/without tocolysis and anesthesia.
Bladder Decompression & Patient Position
The best initial treatment for symptomatic incarceration in the second trimester is bladder decompression combined with a special position of the patient. This treatment brings improvements in most situations. Spontaneous emptying is often impossible, and catheterization is necessary. If the bladder is distended, insert a catheter for 48 hours. If a urinary tract infection is present, appropriate treatment is initiated. During bladder drainage, the patient is instructed to perform repositioning exercises. They consist of adopting the genopathic position every 4 hours for 5 to 15 minutes, with intermittent valsalva maneuver. The patient is instructed to sleep in the pronated position (on the stomach). The spontaneous uterine replacement occurs normally after these steps.
Handling the Uterus
If the above maneuvers prove unsuccessful, a manual repositioning of the uterus is indicated. After an ultrasound, a tocolysis agent is given 15 minutes before reversion. Before the maneuver starts, the woman is instructed to urinate or put a Foley catheter. The patient is placed in a genphatic position. The surgeon inserts a finder into the vagina or rectum, and applies pressure on the incarcerated fundus while simultaneously applying lightweight constant thrusts on the cervix. This combined method will rotate the uterus in the normal position. The maneuver shouldn`t be too difficult for the surgeon or painful at all for the pregnant women.
After the procedure, the ultrasound will be repeated in real-time to evaluate the heart activity and fetal movements. The patient`s symptoms should soon diminish. She is instructed to adopt the genopathic position every 4 hours and sleep in the pronated position to maintain the position of the uterus.
Other Pelvic Malignant Syndromes
Allen-Masters Syndrome
For women who aren`t pregnant, the chronic pelvic pain evaluation that accompanies the retroverted uterus involves the suspicion of 2 different and complex syndromes: pelvic congestion and Allen-Masters syndrome.
Allen-Masters syndrome includes the following elements:
- History of obstetric pelvic trauma.
- Uterine retroversion with hypermobil cervix.
- Cracks in the posterior and subperitoneal fascia of road ligaments.
The symptoms attributed to this syndrome are many and include menstrual disorders, chronic pelvic pain and dyspareunia. Although this cause has first been attributed to obstetric lesions, endometriosis and etiology are suspected. The classical therapeutic approach in these cases consists of the diagnosis established by laparotomy and laparoscopy. Any defects of the peritoneal ligaments are sutured.
Taylor`s Syndrome
Another possible diagnosis is Taylor`s syndrome. This medical condition is represented by menometroragia and signs of continuous pelvic pain. Upon examination, the uterus is soft and enlarged in volume, with a certain degree of sensitivity present. Uterine retroversion is common; the cervix may be cyanotic. Among other therapeutic options, hysterectomy and vascular embolization was used to control the syndrome. The signs are non-specific and poorly defined.
Read more on Pregnancy without Fallopian Tubes: Is this Even Possible?
Is a Tilted Uterus Hereditary?
In many situations, a retroverted uterus is a genetical issue and something completely normal. However, there are also other distinct factors which may cause a retroverted uterus. Like mentioned above, some situations are caused by the labor of birth, endometriosis, pelvic inflammatory disease, pelvic surgery, fibroids or pelvic adhsesions.
410 Comments
viagra without doctor prescription
In 1996, data from 54 published studies on use of the combined contraceptive pill containing an oestrogen and a progestogen in relationship to breast cancer risk were brought together in a pooled analysis 53 cialis otc
generic cialis online Am J Hematol 2018 E202 5
Those seeking to fortify the resistance should not drag it into war between Sunnis and Shi ites finasteride 5mg without a prescription
8 percent from 30 best viagra alternative Patients with endobronchial lesions and interstitial fibrosis also have an un expandable or trapped lung that will render pleurodesis unsuccessful in most cases
viagra • cialis • tadalafil without a doctor’s prescription
buy cialis non prescription Jamar CudcfVfdELvCVugu 6 20 2022
buy cialis 5mg The sinus or fistula tract is dissected with a narrow cuff of normal tissue
cialis and viagra together reddit Egg freezing is recommended for young endometriosis patients because it is minimally invasive and has no effect on future ovarian reserve
563 566, 1991 cialis generic reviews Normal cells expressing CSC markers are associated with cancer risk 140
tadalista vs cialis When used for an extended period of time, this medication may cause a reduction in bone mineral density
ivermectin price canada stromectol for sale
MS1 endothelial cells transfected with Lys179Met Akt mutant showed an Ang1 induced antiapoptotic effect, but the degree of antiapoptotic effect was significantly less than that in the cells transfected with control vector Figure 6 comprare cialis online
These results suggest that DUSP7 might be involved in linc RoR mediated ERK activation in response to estrogen deprivation buy generic cialis online cheap
5 statistical software cialis viagra same time Distribution of TILs in relation to clinicopathological variables
https://stromectolgf.com/# ivermectin coronavirus
cost of tamoxifen Nonetheless, other dosing schedules or routes such as orally may yield different results
is cialis generic galantamine obat apakah bintamox amoxicillin 500 mg Kuperman said the government had made some progress since September 11, 2001, when nuclear plants only had to protect against attacks by three people
Compared with the positive control, all treatments significantly lowered the palpable tumor areas over time and the final tumor volumes and weights at sacrifice cheap cialis In this study, four single nucleotide polymorphisms SNPs rs4753426, rs10830963, rs1562444, and rs1279265 in MTNR1B gene were determined and no differences in genotype and allelotype frequencies for these SNPs were found neither in the PCOS nor in the healthy women
generic ivermectin ivermectin lice oral
cialis online 2004; Hassan et al
Current diagnostics for both metformin for type 1 diabetes diabetes and prediabetes rely on either insulin raises blood sugar levels metformin for type 1 diabetes HbA1c or single time point measurements of blood glucose concentration as such, they cannot describe the nuances blood sugar and pain severity of blank chart for tracking blood sugar How To Prevent Diabetes glycemic patterns women on viagra Net, ASCO s patient information website, to find easy to read summaries of studies that will be presented at this year s Annual Meeting
prix du levitra en evolution Most 60 poison centers had never managed a child at home with charcoal and all 34 of those who had, felt that no adverse events followed
buying cheap cialis online Recurrence after breast conserving surgery A recurrence following breast conserving therapy that is limited to the local regional area around the original cancer is typically treated with a mastectomy
Silencing of Cre lines is likely influenced by environmental factors can you buy viagra at walmart
Mr. Green is a great casino in New Zealand. With the rising popularity of online casinos, Mr. Green has secured a safe place in the rat race. There are thousands of games to play from. The promotions are awesome and the customer support is right on point. Bonuses and promotions are such a big part of playing at an online casino. But are they really worth it..? One of the key factors that most players take into account when deciding which online casino to play at is the welcome bonus offered. Easy way to find information about various welcome deposit bonuses is As far as Mr Green Casino payment options go, players can use Visa, Mastercard, Skrill, Neteller, Paysafecard, iDebit, and a few more. Paypal is not among those options. Players can also use a bank transfer, but, along with iDebit, it’s the option that takes the longest. Go for card payment or e-wallet instead. https://moltingdoc.com/community/profile/agustinziemba39/ Mobile friendly My guest today is Mauricio di Bartolomeo, the co-founder and Chief Strategy Officer of Ledn.io. Ledn provides financial products with a mission to help clients across the globe unlock the power of digital assets to build wealth for the long term. Operating in over 100 countries, … Afficher plus Bitcasino has an expansive, quality casino product featuring more than 2,800 games. Their innovative platform, new features, and rewards are all developed in-house using player feedback to directly shape and create the ultimate user experience. Bitcasino provides an average withdrawal time of around one-and-a-half minutes, among the fastest in the industry, and cutting-edge security measures. Sie kГ¶nnen Ihre Gewinne in sechs verschiedenen KryptowГ¤hrungen abheben, darunter mehrere beliebte KryptowГ¤hrungen: BTC, ETH, LTC, TRX, XRP und Keno Online Casino. Was mir im Bitcasino Test gefallen hat: Ihr kГ¶nnt die RTP-Werte aller Bitcasino Review im MenГј einsehen.
To assess LC specific survival, Kaplan Meier analyses were performed separately for women diagnosed with LC within or after the first year from BC diagnosis buy cialis pills
cialis online reviews In this, your husband produces a semen sample by masturbation and the doctor treats and inserts the sample directly into your uterus
The cisplatin leaves her feeling lousy, but she suffers no side effects on the day she receives taxol tadalafil cialis from india Similarly, there was no excess breast cancer risk associated with clomiphene, human chorionic gonadotropin, gonadotropin analogues and progesterone when examined individually
Common Patterns of BPE buy generic viagra online viagra para que sirve el betnovate crema We ve started strong, said Covered California Executive Director Peter Lee
That was the worst part buy cialis online using paypal
20 off coupon code LEAVINGWEAKNES buy cialis online europe But after that and over the years, my period has basically disappeared, to where I only spot have small period on the 2 weeks before my next shot is due
buy sumatriptan online – purchase imitrex without prescription sumatriptan 25mg price
Research peptides claims to offer peptides at low prices cialis pills
PubMed 12055601 buy cialis online with a prescription Multivariable Cox proportional hazard regression models were used to identify prognostic factors, and the results were reported as hazard ratios HRs with 95 confidence intervals
where can i buy priligy in usa Mice are nocturnal and will spend most of the day sleeping
OXA, TEM, and SHV hits were investigated differently cheapest finasteride on the web
Cryptocurrency is a collection of binary data designed to work as a medium of exchange over the Internet and used outside existing banking and governmental institutions. More… Don’t be careless: Crypto news site CoinDesk has a guide on how to spot the scams, including how to reach out to their in-house experts for help. If you plan to invest, at least go in eyes wide open. Ethan WuThere’s no specific reason. Terra luna crashing should cause tether to unlink, but crypto is a lot about vibes. It’s about sentiment. It’s about how people feel. When people get scared, they run for the hills. And I think that’s really what you saw is, you know, terra luna crashed and people were like. Like, Oh, crap, you know, is this a broader problem in stablecoins? And they started selling their tether. But I think the fact that tether bounced back within an hour or two shows that it really was kind of like a temporary worry rather than like a fundamental fear that tether’s reserves are like like bogus or garbage or whatever. https://abbatrust.org/community/profile/tamerasinnett0/ Network fees are paid to cryptocurrency miners, who process and secure crypto transactions on the blockchain. Many centralized crypto exchanges incur this cost, though some may allow their users to pay more in miner fees to speed up transaction speeds. Users on decentralized exchanges generally have to pay this themselves, since there is no third party between them and the crypto miners. Please enable Cookies and reload the page. In addition to delivering access to the largest cryptos by market cap, Crypto.com also gives investors access to the lesser known cryptos. This gives investors opportunistic income from cryptos that have yet to hit the mainstream. On August 24, 2020, a day the city of Los Angeles designated Kobe Bryant Day to honor former Lakers guard Kobe Bryant who died in a helicopter crash in January of that year, the City of Los Angeles announced that Figueroa Street between Olympic and Martin Luther King Jr., which includes the area Crypto.com Arena is on, will be renamed Kobe Bryant Boulevard.
of patients Contralateral prophylactic mastectomy No 69 69 Yes 31 31 Age at diagnosis 42 years 52 52 42 years 48 48 Ashkenazi Jewish ethnicity AJ No 89 89 Unknown 2 2 Yes, unspecified 1 1 Yes, paternal side 3 3 Yes, both sides 5 5 Race Unknown 2 2 AJ White 9 9 Black 5 5 Non AJ White 68 68 Others 16 16 Marital status Unmarried 25 25 Married 75 75 Education Advanced degree 24 24 College 31 31 Some college technical school 23 23 High school 11 11 Less than high school 1 1 Unknown 10 10 First degree family history of breast cancer 0 57 57 1 43 43 Total no 5 mg cialis generic india marketand reuniting a substantial portion of the Del Monte brandfamily
How do you deal with the grief of infertility, altered body image, scars, pain, premature menopause, or the financial difficulties and trying to go back to work buying cialis online forum
cialis for sale online With a better understanding of how sex influences disease and immunity, we can envision sex specific therapies to better treat diseases of the urinary tract and potentially diseases of other mucosal tissues
2 mg kg week equivalent to 0 prix levitra pas cher
2011; Donoso et al buy cialis 5mg
The existence of these black qi prevented the normal blood pressure and caffeine Recalled High Blood Pressure Meds operation of her spiritual power viagra and alcohol interaction Chemotherapy is any treatment involving the use of drugs to kill cancer cells, and is a standard adjuvant therapy for the treatment of early stage breast cancer
Bei einer Auszahlungsquote von 96,86 % und gleich 4 unterschiedlichen Freispielrunden, die Sie nach und nach freischalten, überrascht es nicht, dass Immortal Romance seit Jahren ein Favorit von Online Casino Spielern ist. Hierbei kommen dann fГјr die Top-Ligen Auszahlungsquoten zwischen 95% und 97% heraus – je nach Buchmacher. Mit Sportwetten hat man also recht gute Gewinnchancen. Statt der bislang in GaststГ¤tten erlaubten drei GeldspielgerГ¤te, dГјrfen in Zukunft nur noch zwei GerГ¤te pro Betrieb aufgestellt werden. Viele GeldspielgerГ¤te verfГјgen Гјber eine sogenannte Automatiktaste. Mit dieser Taste werden ohne Zutun des Spielers EinsГ¤tze getГ¤tigt. Spielen Sie so viele Gewinnlinien und mit so vielen Features wie möglich. Spielautomaten sind beliebt. Leider gehГ¶ren sie aber auch zu den riskantesten und am wenigsten beeinflussbaren GlГјcksspielen bzw. Automaten. Viele Spieler sind der Meinung, dass Sie mit der richtigen Spielautomaten Strategie die Automaten manipulieren kГ¶nnen, da die Walzen nach einem hinterlegten Zufallsprinzip stoppen. Leider ist das nicht der Fall. Alle Slot-Automaten basieren auf voreingestellten Wahrscheinlichkeiten, so dass kleine und mittlere Gewinne wahrscheinlicher sind, als die MГ¶glichkeit groГџe Gewinne oder gar den Jackpot abzurГ¤umen. Der Ablauf des Spiels wird bereits beim ersten Druck auf den AuslГ¶ser entschieden, das Warten, Drehen und Blinken sind lediglich Show. https://collinzarg310865.blazingblog.com/12387374/casino-merkur-online-kostenlos Der beste Preis, der bei Book Of Ra Magic Slot gewonnen werden kann, ist 5.000 MГјnzen, und das ist erlaubt, wenn eine mit Pionierbildern gestapelte Sieglinie ausgelГ¶st wird. Die Summe in zertifiziertem Geld, die dieser 5.000-MГјnzen-Rieseneinsatz wert sein wird, hГ¤ngt von der Bewertung Ihres Einsatzes ab, also je mehr Sie setzen, desto mehr werden Sie gewinnen. Der NOVOMATIC AG-Konzern ist mit rund 1,8 Milliarden Euro Umsatz im Jahr 2021 einer der größten Gaming-Technologiekonzerne der Welt. Die im Jahr 1980 gegrГјndete Unternehmensgruppe verfГјgt Гјber Standorte in rund 50 LГ¤ndern und exportiert Hightech Gaming-Equipment in rund 100 Staaten. Ja! Book of Ra kannst Du ohne Download einer Software und ohne Registrierung kostenlos spielen. Du spielst mit Spielgeld ohne echten Einsatz und das 24 Stunden 7 Tage die Woche, rund um die Uhr.
2017 Jan; 22 1 12 17 cialis without a prescription Luckily his sample was taken at a different facility and they did a fantastic job explaining the analysis
66 ng mL, respectively, on Day 1; and 204 where to buy viagra connect usa Per the NCCN guidelines 7, none of these men should have received bone imaging unless they presented with symptoms suggestive of bone pain 8, 24
No Susquehanna Join Date Oct 2003 Location Tulsa, Oklahoma, United States Age 40 Posts 6, 795 Rep Power 2802 will 10 year old viagra work In sensitivity analyses, we examined other choices of weights
More than 50 of women don t report vaginal dryness to their healthcare providers, and fewer than 4 of women affected are using any proven therapies to counteract their symptoms viagra reviews forums
онлайн кино смотреть
generic cialis 5mg While machines do provide sufficient stimulation to gain muscle, nothing can beat free weight compound exercises
Palbociclib shows promise as mono or combined therapy in myeloma, non Hodgkin lymphoma, lung cancer, colorectal cancer, and melanoma cheap cialis online PubMed 9460178
best price for generic cialis Drugs 48 431 454
can women take mens viagra Plasma ctDNA analysis revealed ESR1 mutations in 30 of patients at study entry, consistent with heavy pretreatment with aromatase inhibitors
Bok has previously been shown to be EE responsive in uteri, whereas Pdcd6 approached the statistical cut off in a previous study 15 finasteride propecia PMID 33833678 Free PMC article
Kisspeptin neurons in the ovine arcuate nucleus and preoptic area are involved in the preovulatory luteinizing hormone surge cheapest place to buy cialis 239 263 in Estrogens in the Environment
Med Case Rep Vol basf levitra 20mg
First, it’s essential to find a therapist who is experienced in sports massage. They will know how to target the muscles most likely to be tight and sore after your workout.
cialis online without prescription Shavell is very knowledgeable and kind
levitra costo Description Estimated percentage of patients alive and disease free at 5 years from randomization, where disease free survival is defined as the time from randomization to the first appearance of one of the following invasive breast cancer recurrence at local, regional, or distant site, invasive contralateral breast cancer, second non breast invasive cancer, or death without cancer event; or censored at date of last follow up
is viagra a vasodilator Diuretic doses should be titrated as necessary Figure 6, Table 7
He was attacked by another prisoner while talking to a friend on the telephone generic 5mg cialis best price
buy cialis online without a prescription Ann Oncol 2 347 354
Be careful and be sure to specify the information on the section Preclinical safety data in the instructions to the drug Tamoxifen Nichi iko directly from the package or from the pharmacist at the pharmacy order cialis
buy cialis usa Driscoll GL, Tyler JP, Hangan JT, Fisher PR, Birdsall MA, Knight DC
ivermectin stromectol scabies Achat Malegra
brand cialis online Based on our analysis, we also hypothesize that D309 is involved in the irreversible binding of exemestane intermediates
generic for cialis Lacquer tree, Rhus verniciflua 1
Then I couldn t handle the side effects so I stopped taking it which upset my Onc Doc finasteride without prescription uk Dennis XhvVOxBQxSgCN 6 27 2022
Clair OkACvMqKUVc 5 20 2022 will customs seize viagra
Drug interactions with doxycycline monohydrate oral and phenytoin oral cialis online ordering
Please let me know if you’re looking for a author for your site.
You have some really great articles and I think I would be a
good asset. If you ever want to take some of the load
off, I’d love to write some articles for your blog in exchange for a link back to mine.
Please send me an email if interested. Thank you!
where to buy clomid online bodybuilding I wish we had moved faster to help, but I had a romantic idea of how it was going to go
We compared two review methodologies one included and the other excluded high quality case reports studies and case series generic cialis tadalafil
Inpatient hospice centers can be found in larger cities in the United States as well, but a majority of the care is provided in the patient s home, or the home of a caregiver or loved one if the patient is staying there hair loss propecia mastigra ibuprofen und paracetamol im wechsel kinder It will also raise the comfort levels of companies supplyingthe content to a mobile commerce sector expected to reach 40billion next year in the United States alone, according toEuromonitor estimates
prix levitra 20mg france The Reverse Effect Vegetative Reflex Diagnostics letter 130, p
These TrussRod Covers are made of 2-Ply ABS Plastics, include mounting screws, and are 100 made in the USA online generic cialis
These are the vaccinations we have best place to buy generic cialis online WDR5 has multiple functions in chromatin mediated gene regulation and is best known as a core component of the mixed lineage leukemia MLL histone H3K4 methyltransferase complex together with ASH2L
The approach to the ear can be transcanal, endaural, or retroauricular cheap cialis online pharmacy
What I don t value is people not contributing their opinions and instead merely critcizing those that do finpecia tabletten Grunebaum A safe uncomplicated abortion in the past won t affect your fertility at all
The problem of not able to make out with the partner is referred to as Erectile dysfunction cialis online Blink Health Best for All-in-One Service At Blink Health, you simply set up an account to complete a consultation and prescription order all at one time
Thus, we can conclude that the capacity of GPR30 to mediate estrogen action is significantly reinforced during development of tamoxifen resistance in breast cancer cells generic cialis online pharmacy Loosen clothes and apply cool, wet cloths to the neck, face and arms
Longwei made all the horses terrified, and they all stood up and turned around natural alternative to lower blood pressure and ran buy generic cialis online cheap Avoid exposure to intense light
If not A to Z, they do run from Clomid to Vivelle, and beyond cialis prescription online Senior brother, have you also lost Xuan Linger was not in front of Bai Tu just now, so she did not see how Bai Tu lost, and asked directly
Blood tests are often used in combination with other clinical assessments and tests to diagnose pancreatic cancer viagra vs cialis
Tadarise 10 Mg 20 Mg 40 Mg Tadalafil Tablet Usp buy priligy online safe
cheap cialis Fast acting and long lasting Testosterone enantate Moderate androgenic properties; in an injectable oil preparation
Fig 3 shows data from the experimental series in which we tested the effect of luminal furosemide at 50 Ојmol L on the NaCl dependency of renin secretion precio priligy 30 mg And I think the conference commissioners that I ve spoken with throughout the range of Division I are open for that discussion
Previous studies have identified that PI3K inhibition can reduce GATA3 protein expression in T cells and prostate carcinomas 34, 45 order priligy online uk
Drugs can be abused in the following ways cheap propecia online uk
priligy 30 mg Third is determination of individualized treatments for influenced people
Since the C6 signature is characterized mainly by low grade endometrioid tumors, which were not present in our cohort, this finding supports the ability of gene signatures to capture histological differences, and indicates that the C signatures are stable and widely applicable across datasets and microarray platforms cialis online no prescription
A friend of mine who has endo used clomid and she ended up having twins levitra boutique After its removal, fertility should return within one month s time
Featured Centers priligy over the counter 0 , continued TAD-OaD at Month 6
In previous studies, our group first cloned the CLDN6 gene from mammary epithelial cells of COP rats and identified CLDN6 as a breast cancer suppressor gene 18, 19 buying cialis online safe Roderick mUvSBuvekYKThl 5 29 2022
generic cialis 20mg Yýldýz N, Sever L, Kasapçopur Ö, Çullu F, Arýsoy N, Çalýþkan S
generic for cialis I ve never miscarried before
Bevacizumab was given at 15 mg kg every three weeks levitra dosage 20mg
For me it s not the coffee as It doesn t happen on all the other days that I have just breakfast and a coffee can i buy cialis without a prescription
This institution is an equal opportunity provider buy cialis 20mg If I use 10mg
PMID 2431543 Review does tamoxifen cause menopause Next, we explored the transcriptional changes associated with the R14del mutation
taNK, Adjuvant Dendritic Cell immunotherapy, D CIK, DOT Cells, Autologous Tumor Lysate TL plus Yeast Cell Wall Particles YCWP plus Dendritic Cells, Autologous EBV specific Cytocytotoxic T Cells, Autologous TLPLDC vaccine tumor lysate, particle loaded, dendritic cells, Regulatory T Cells, Personalized Cellular Vaccine PERCELLVAC, CAR pNK Cell, HER2 cialis 5mg online
order cialis online During POR, no significant difference was observed not shown
buy cialis with paypal But is it legally OK to do this, and are the drugs safe
35, 63 72 2003 cialis on line Dghonson OvpVGryqcTeeDoSdc 5 19 2022
Elevated progesterone during ovarian stimulation for IVF buying generic cialis online safe The authors also compared AUC 0 360 ratio of the brain interstitial fluid and plasma for all 9 molecules after IV infusion 1 mg kg h for 6 h or 3 intermittent doses of IP or SC injections 2 mg kg, every 2 h 66, 67, 68
1021 ic902176e PMID 20199051 priligy review It is at Helix MWR s discretion to decide what a patient s payment will go towards in terms of covering services
In CKO embryos with cleft face, the nasal capsule failed to fuse, and the palatal shelf asterisk failed to form levitra en andorra
2012; 7 1 47 70 buy cialis generic online
Buy Viagra and Cialis in Jacksonville, Florida buy generic cialis online cheap
cialis otc swollen feet, ankles, legs, etc
You need to have someone drive you there and drive you back home, because you won t be able to see for that afternoon viagra pill price
Therefore, at this point, AIs are not recommended to treat patients with late onset hypogonadism buy cialis online
how long do viagra last Rosenberger C
Provided input and direction in scientific forums about areas conducive to research partnerships with Alaska Natives and highlighting needs for new or expanded research buy cialis online with a prescription
Jacob ODzvCybwxYW 5 20 2022 canadian pharmacy cialis Intravenous diltiazem 10 mg was administered for rate control
cialis super active New York, NY Springer Verlag; 2017
This work was supported in part by Grants in aid for Scientific Research from the Ministry of Education, Culture, Sports, Science, and Technology of Japan propecia cost
67 MEQ ML Oral Solution Potasio Cloruro Corpaul Potassium Chloride 0 cialis pills
Additionally, if a man using testosterone replacement therapy discontinued their medication, their levels of testosterone would immediately drop and their body would have to restart making its own testosterone. can clomid delay a positive pregnancy test With proper counseling and care, the chances of getting pregnant with endometriosis are high for most women.
dicyclomine decreases levels of chlorpromazine by pharmacodynamic antagonism buy cialis canada pharmacy
cialis generic reviews Cross- fertilization would mean lost sales forconventional and organic growers businesses, they said
For example, the percentage of large employers who require employees 55 years or older to have between 10 and 15 years of employment to qualify for benefits rose from 30 percent in 1991 to 49 percent in 1998 cialis and viagra sales The 21 year old came into the UAE on her Danish passport, as traveling on an Israeli one remains complicated despite moves by the two countries to start telephone service and other outreach
UUU Stinging insects; viagra pill cost
The process is less demanding on the body and offers a clear visual representation of the uterus, allowing a specialist to see any abnormalities within it. online doctor to prescribe clomid
48 6396 1988 buy cheap cialis discount online 3 8 Goldenhar syndrome was considered to be a variant of HFM, characterized by additional anomalies of the ribs and vertebrae and the presence of epibulbar dermoids
buy cialis 5mg daily use Likely the concept of tumor targeting, Gharib et al
is cialis generic Mathieu Neault,
Thus many breast cancer patients taking TAM report increased use of complementary dietary supplements including phytoestrogen rich foods such as soy and FS, instead of taking hormone replacement therapy, to reduce menopausal like symptoms and also to supplement the tumor reducing effect of TAM 14 organic viagra
Handicapping should be done in a quiet place before the races begin online cialis pharmacy atazanavir decreases effects of miglitol by Other see comment
Why are they making you wait so long doing nothing. how quickly can tamoxifen cause uterine cancer
is 80 mg of accutane a high dose nitrofurantoin yellow pill gabapentin Гў
viagra and cialis online Antiestrogen therapy uncertainties and risk assessment
Kari JA, El Morshedy SM, El Desoky S, Alshaya HO, Rahim KA, Edrees BM 2011 Rituximab for refractory cases of childhood nephrotic syndrome cheap cialis generic online
nolvadex pct for sale In contrast, in the study reported by Legro et al.
Cognitive function has been reported to be affected in IIH 59 buying cialis online reviews
Why Use Novaldex for Cutting where to buy cialis Since we had already gone the pill route only to have the fungus return, I figured what could be the harm of giving it a try
meilleur viagra cialis levitra 97 compared with noncarriers
As it is not as powerful as its brother compound Nolvadex buy priligy without a script
propecia finasteride Trimethoprim alone bactrim negative in in vitro reverse mutation bacterial assays and in in vitro chromosomal aberration assays with Chinese Hamster ovary website lung cells with or without S9 activation
buy doxycycline Nude mice strain CD- 1nuBR, up to 6 8 weeks old were obtained from Charles River Laboratories, Inc.
is 80 mg of accutane a high-dose This drug combination has also shown to reduce the rate of brain metastases as the first site of progression from 6 with capecitabine alone to 2 with capecitabine and trastuzumab P 0
safe place to buy cialis online Monitor Closely 1 mifepristone will increase the level or effect of amlodipine by affecting hepatic intestinal enzyme CYP3A4 metabolism
After a breast cancer diagnosis, one of the most important decisions you ll make is choosing your treatment team achat 20mg levitra en france
dose of doxycycline for pneumonia No one I ve consulted at the aquarium stores has a guess at this point and you are the best.
Make money trading opions.
The minimum deposit is 50$.
Learn how to trade correctly. How to earn from $50 to $5000 a day.
The more you earn, the more profit we get.
binary options broker
It is not known whether Tamoxifen Sawai passes into breast milk or if it could harm a nursing baby generic 5mg cialis best price Understanding the reasons will be beneficial for treating women with lung cancer in the future
Even in my worst case scenario, I didn t imagine how bungled the process would turn out to be how to buy priligy as a child
best place to buy cialis online forum Do not utilize aggressive fluid therapy for rehydration
How does blood pressure affect my health cialis professional Feeling cold, particularly in the hands and feet
com 20 E2 AD 90 20Como 20Puedo 20Hacer 20Viagra 20Casera 20 20Viagra 20Vid 20Hgt 20Blodtryck como puedo hacer viagra casera Following Romney s loss, in which Republicans lagged far behind in support among women and minority voters, some party leaders have engaged in soul- searching, looking at whether some Republican positions have become too conservative to appeal broadly to voters is there a generic cialis available
finasteride propecia If a Canadian Pharmacy Propecia finds be generous and thoughtful has no clickable definition gear on our current allowed us inside his
levitra impuissance Our central hypothesis is that forward screens performed using our zebrafish model of MYC induced T ALL will lead to the identification of entirely novel genes and pathways that play critical roles in MYC induced leukemogenesis
Howdy! I could have sworn I’ve visited this blog before
but after going through many of the posts I realized it’s new to me.
Regardless, I’m definitely delighted I stumbled
upon it and I’ll be book-marking it and checking back
often!
cheapest propecia uk Severe interactions of calcium acetate include demeclocycline lymecycline oxytetracycline
I am starting this herb, soon instead of the harmone blocker I am on propecia walgreens
Brand name and generic companies will need to be prepared to justify their settlement agreements pills like viagra
buy generic cialis online safely Jarrett nZsjxWSxkENBUKSI 5 29 2022
Clarus Eye Centre serves Lacey, Olympia, Tumwater, and surrounding areas in Washington state cheap cialis online canadian pharmacy
best datings sites free dating online fdating international https://adult-classifieds-online-dating.com/?singles%20to%20meet
The self proclaimed meatball has slimmed down in recent years after jumping into the reality TV limelight generic cialis 5mg The treasure that was teleported to Artest, the great general of the demon world
So they compared the outcomes of the 324 women in the BIG 1 98 study diagnosed with lobular breast cancer to the 2, 599 women diagnosed with ductal cancer who got only Femara or only tamoxifen cialis viagra combo pack Patients who were diagnosed as H
Follow pre op instructions to the letter Follow all post op instructions to the letter Carry lubricating eye drops with you at all times especially in early months after surgery Avoid smoking and smoky environments Be wary of dusty, dry, or pollen filled places buy generic propecia online Generally, in the ED, the goals can be classified as
What i do not realize is if truth be told how you
are not really much more well-liked than you might be right now.
You’re very intelligent. You know thus significantly in relation to this subject, produced me individually believe it
from numerous various angles. Its like men and women don’t seem to be interested except it’s one thing to do with Girl
gaga! Your own stuffs outstanding. At all times maintain it up!
Innumerable fashions are an appraised value for you know if the antidepressant now real cialis online Medications for the treatment of medical conditions that can cause heart failure or make the condition worse, such as atrial fibrillation, high blood pressure, diabetes, obesity, coronary artery disease, chronic lung disease, high cholesterol and kidney disease
59, 60 All treatment options are controversial cialis otc Crizalk 250 mg Capsules
His family history was non contributory; he lived with his family, had a regular job, and used to engage in physical activities daily cialis 20mg Absence of KLF5 inactivates numerous selected enhancer elements and direct transcriptional targets including canonical WNT and NOTCH responsive genes
Cells were plated evenly in control and experimental wells, were allowed to grow to log phase and were then treated with 100 nM PD 0332991 for the defined times what is lasix
how to buy cialis Elevated Blood Pressure
ASA, an anti inflammatory cyclooxygenase COX 1 and COX 2 inhibitor, 22 has been repurposed as an anti cancer agent given its broad efficacy in regulating the hallmarks of cancer best place to buy cialis online reviews
buy finasteride 5mg with amex While this kind of genohype has been a concern for stakeholders, including policymakers as they attempt to reconcile it with the pressures of a constrained health service, such expectations for genomic medicine have also been recognised as a stimulus and as necessary to drive clinical change Samuel and Farsides 2017
As in complete AVSD, take care to avoid injury to the conduction system, often by closing the coronary sinus into the left atrium order cialis
blue generic viagra pills lidocaine ciprofloxacino ratio Saturday s ballot was the sixth since 2006 in the major oil producer where political upheaval and bureaucracy have held up the vast majority of projects in a 30- billion- dinar 105- billion economic development plan announced in 2010
lasix iv to po Wilson, continues to wage her own battle against a prison system that she says has left her body ravaged and disfigured by breast cancer
Everyone knows what they should know in their hearts, and they weight loss diet can come up with theories on the table, Then, Liu Zi trotted back golo weight loss quickly and said General, I have lose weight fast adkins already asked weight loss plan la shape diet best foods to eat when trying to lose weight the matter clearly cialis tadalafil By using the database of Yale New Haven Hospital, we collected and analyzed a significant number of cases over an extensive period of time and thereby our study population constituted an adequate representation of the general population in respect to the morphological parameters we investigated
buy cialis online prescription observed significantly changed levels of amino acids, acylcarnitines, glycerophospholipids, sphingomyelins, and the sum of hexoses, with average increases or decreases of 13
I have long, thick hair also and go through the same conundrum you discuss here on how much easier and less expensive those shampoo bottle are supposed to suds up more than one shower worth cialis coupon Prevention and management of adverse events related to regorafenib
priligy farmacias del ahorro Thyroid function in patients with nephrotic syndrome and normal renal function
Wow, amazing weblog structure! How lengthy have you been blogging for?
you make running a blog glance easy. The entire glance
of your web site is fantastic, as smartly as the content material!
E Representative genes that were exclusively upregulated in esophageal eosinophils compared with bone marrow eosinophils from CC10 Il13 Tg Pirb mice buy cialis usa As with other antimicrobials, prolonged use of cefazolin injection may result in overgrowth of non susceptible microorganisms
Kotilainen, S buy cialis 5 mg vial Injection, powder, for suspension, extended release; kit Intramuscular 50 mg 2mL Injection, powder, for suspension, extended release; kit Intramuscular 50 mg vial Injection, powder, for suspension Parenteral 50 mg Injection, powder, for suspension, extended release Parenteral 25 mg Injection, powder, for suspension, extended release Intramuscular Injection, suspension, extended release Intramuscular Injection Intramuscular Injection, powder, for suspension, extended release Parenteral 37
The show is like an ordinary plant show, with some amazing specimens diplayed on long tables, and labelled cialis 10mg As muscle length was fixed in all experiments, and muscle density is assumed to be a constant, physiological CSA of the TA was solely a function of muscle mass
The possibility of increased risk for osteoporosis in breast cancer patients treated with tamoxifen was investigated real cialis online Intervention s Patients received anastrozole 1 mg d; 115 patients, 243 cycles for 5 days, starting on day 3 of menses
Tetracyclines are commonly prescribed for a 7 day course, with reports that longer courses do not change outcomes finasteride vs propecia 24 and fell to 1
смотреть фильмы онлайн музыка сериалы видео
Since the dosage was low and the cycle short, anti estrogens were not utilized nor was there need for HPTA stimulating compounds post cycle buy cialis usa 2009, 13 R104 10
Other studies have reported that astaxanthin reduces Adriamycin induced heart damage in rats cialis 5mg Testing for infertility usually begins with a nurse or doctor talking with you about your medical history and doing a physical exam
Dearest Susun, Thank you SO much for answering my email cheapest propecia uk
soft tab cialis AMERICAN JOURNAL OF THERAPEUTICS, 2016
Welcome to Fertility Solutions interactive session on PCOS and treatment options beyond clomid buy cheap generic cialis online Claire wKOGhSLfAdFHer 6 28 2022
comprar levitra barata 1 of patients were diagnosed as HER2 positive
To maximize the body s production of collagen, some of these foods contain protein and anti- aging nutrients that are good for preventing premature aging, including cow s milk, edamame, red quinoa, macadamia, and garlic buy generic viagra
Türkiye Haberleri
Thus, we examined whether generating physiological levels of cAMP by Golgi bPAC can phosphorylate and activate downstream targets of PKA buy azithromycin without prescription But it had been set ablaze
cialis generic tadalafil Brains were removed and postfixed with 4 PFA in PBS
Figure 1 Generation of a conditional C xcr 2 allele and genotype determination of conditional knockouts by PCR medicamento priligy estudios clinicos
generic cialis vs cialis It would take more universes than 6 times the number of atoms in the observable universe
I ve had a few cases where it has been green or blue in the tattoo cialis generic best price These results account for the previous observation that vasopressin increases the apical potassium conductance
Thus, in addition to the hyperplasia inducing capability of an estrogen mimetic, tamoxifen has an additional tumor promoting capability similar to that of TPA cialis buy
My breast are starting to feel tender as well, so maybe it is just mentral pain generic lasix no prescription
While glatiramer acetate has been used for over two decades in the management for multiple sclerosis, overt hepatotoxicity appears to be quite rare real cialis no generic Common Parlodel and Clomid drug interactions by age
02 2 5 Oligoadenylate synthetase like Homeostasis STC1 AI300520 0 cheapest cialis Monitor Closely 1 iodine radioactive decreases effects of heparin by pharmacodynamic antagonism
16 In fact interest in the micro flora of root canals has largely been focused on anaerobic bacteria due to their predominance in untreated canals levitra 20mg cout A larger study by Yang et al
Impact of Amlodipine on Other Drugs Simvastatin Coadministration of simvastatin with amlodipine increases the systemic exposure of simvastatin how much does cialis cost
generic cialis 5mg Join us on 5 17 from 4PM as the Virginia Diner celebrates the powerful mission of the James House and the work that it does to lift others in our community
Effects on angina cialis prescription online Many over the counter pain relievers belong to the same class of drugs as meloxicam, including aspirin
She was alert and oriented but unable to recall events from earlier in the day buy cialis online usa Edison cthWJxJSXzFsdnxAlD 6 28 2022
I don t know what that is cialis online reviews
how much does cialis cost desipramine and clarithromycin both increase QTc interval
Thank you for sharing your thoughts. I truly appreciate your efforts and I will be waiting for your
further write ups thank you once again.
Estrogen receptor alpha forms estrogen dependent multimolecular complexes with insulin like growth factor receptor and phosphatidylinositol 3 kinasein the adult rat brain buy cialis online safely The often quoted saying Aging isn t for sissies is so true, but cancer forces aging
Pathology, Hospital israelita Albert Einstein, SГЈo Paulo, Brazil discount cialis Within minutes he injected 1 mL of polyvalent antivenom Instituto Clodomiro Picado Polyspecific, Costa Rica at the bite site
What s your success rate for assisting couples in achieving pregnancy nonprescription levitra Forty percent of clomid at higher bmi over a lot of an unhealthy manner, 2017
3 From my research Proviron increases free test by lowering shbg is propecia from budgetmedica real This work was supported by grant 1132 from Teva Pharmaceuticals Ltd that was awarded to Salomon M
conjugated amoxicillin and tylenol cold and flu Two women from Pussy Riot are serving two year jailsentences for hooliganism motivated by religious hatred for the punk protest, which the head of the Russian Orthodox Churchhas called part of a campaign to curb its post Soviet revival does viagra make you warm If it doesn t go away which can happen in very rare cases, talk to your doctor
000 500 mg Caja x 30 tabs zithromax azithromycin Some or all the survival advantages that younger women with ER HER2 tumors derive from chemotherapy may be because of the suppression of ovarian function, which occurs as a side effect of chemotherapy
Step 7 S, E N 4 S 2 S 2 Amino 3 methylbutanamido 5 ureidopentanamido methyl phenylsulfonyl 2, 5 dimethyl 4 S N, 3, 3 trimethyl 2 S 3 methyl 2 methylamino 3 phenylbutanamido butanamido hex 2 enamide levitra que es yahoo cialis clindamycin and benzoyl peroxide cream Yes, the exploration of the universe has been declared non essential
The percentage of patients reporting symptoms of sexual dysfunction in males and females with MDD, OCD, PD, SAD, GAD, and PTSD are displayed in Table 8 arimidex vs nolvadex
propecia dosage Lots of people don t have any direction or focus when they start their career and they just drift from place to place
buy nolvadex This work in diffuse large B cell lymphoma, published in Nature in 2000 and validated in the New England Journal of Medicine in 2002, was the first to segregate clinically and molecularly distinct subtypes of diffuse large B cell lymphoma based on gene expression
Thanks for ones marvelous posting! I genuinely enjoyed reading it, you might be a great author.
I will ensure that I bookmark your blog and will eventually come back from now on. I want
to encourage you to continue your great job, have a nice
holiday weekend!
Woah! I’m really loving the template/theme of this site.
It’s simple, yet effective. A lot of times it’s challenging to get that
“perfect balance” between superb usability and visual appearance.
I must say you have done a very good job with this. Additionally,
the blog loads super quick for me on Firefox. Exceptional Blog!
https://drugsoverthecounter.com/# strongest diuretic over the counter
Hello pregworld.org owner, Your posts are always informative and up-to-date.
2226 N California Ave, Chicago, IL 60647 773 235 2663 clomiphene citrate over the counter 00093 7306 Celecoxib Teva Pharmaceuticals USA, Inc
how much does clomid cost While fortunately, most athletes are aware of the side effects of Steroids, including hair loss and impotence, Creatine s side effects are not as much discussed
accutane dosing calculator Slides were incubated in hybridization buffer 50 Formamide, 5 SSC, 50 Ојg ml Yeast tRNA, 100 Ојg ml heparin, 1 Denhardt s Solution, 0
The susceptibility rate of toxigenic C clomid by avents The best way to minimize these reactions is strict sun protection and avoiding excessive sun exposure, says Dr
accutane birth control Efficacy in terms of improvement of exercise capacity or pulmonary hemodynamics has been shown in primary pulmonary hypertension and pulmonary hypertension associated with congenital heart disease 15
where to buy cialis online forum When used medically though, a moderate amount of hydrocortisone is supplemented to avoid this reaction
where to buy zithromax online viagra clindamycin topical pregnancy For example, if it determined that the user of the mobile computing device is moving, for example, the user is driving, then the messaging applications may change the users preferred communication method
Patient and family history can be helpful, and specialized tests may help to exclude certain disorders with similar symptoms buy cialis online safely
Is it fine to stick to the 1 day refeed or would there be any benefit to fat loss with two day refeeds aside from the momentary pleasure of eating carbs buy zithromax
and Raison Peyron, N acne accutane
The major macular disease which we know more about is age related macular degeneration ARMD for which the NIH has guideline to help protect the macula including oral supplements of lutein and zeaxanthin dose of clomid
Analyses of public microarray methylation data showed that TAGLN was also hypermethylated in 63 how to order clomid on line in canada This antibiotic class consists of four major groups penicillins, cephalosporins, monobactams and carbapenems
Lapuk A, Marr H, Jakkula L, Pedro H, Bhattacharya S, Purdom E, Hu Z, Simpson K, Pachter L, Durinck S, Wang N, Parvin B, Fontenay G, Speed T, Garbe J, Stampfer M, Bayandorian H, Dorton S, Clark TA, Schweitzer A, Wyrobek A, Feiler H, Spellman P, Conboy J, Gray JW Exon level microarray analyses identify alternative splicing programs in breast cancer propecia success rate
anastrozole online arimidex 1 mg cheap oral arimidex 1 mg
clomid for men Apolipoprotein A I ApoA I was identified using a rabbit polyclonal anti ApoA I antibody from Santa Cruz Biotechnology Inc
20 mg nolvadex pct Lancet 347, 1351 1356 1996
wonderful issues altogether, you simply received a new reader.
What could you suggest about your submit that you just made some days in the past?
Any sure?
Previously, I only felt the community of software testing at the conferences I attended or phone calls with people in our field is tamoxifen chemotherapy
J L Protein immunohistochemical results of PI3K in lung tissues in female mice kamagra kent
Free video poker is fun, but nothing beats the thrill of winning cash when playing video poker games for real money. You can enjoy the best quality poker slots at our premium real money Canada casinos, while also taking advantage of bonuses to spice up your gameplay. Choose a Canadian casino site from our expert list above, or get your video poker journey started instantly by joining our #1 casino below: In a similar vein, Parx values slot play far more than video poker play. Rather than any sort of calculation, Parx’s Xclub awards 1 point per $20 wagered on slots and 1 point per $60 wagered on video poker. So, playing video poker is a third less fruitful than playing slots. Video poker is one of the most common games at brick-and-mortar casinos. As mentioned above, almost every bar top in Las Vegas has built-in video poker tables. But all casinos across the US have video poker unless it’s specifically prohibited by law. For example, card rooms in California can’t have video machines, which include both slots and video poker.
https://picomart.trade/wiki/Sun_palace_casino_no_deposit_bonus
It’s believed that the game of blackjack has its roots in France. It was originally known as 21. The goal of the game is to beat the dealer’s hand by scoring 21 or as close to 21 as you can get without going over. If the dealer scores closest to 21, you lose. When playing blackjack there are two options – to hit or to stand. Consider this: all rules being the same as other RTG blackjack games, Match Play 21 stretches payout odds-and opportunities-by using the cards you’ve already been given and making them work harder for you. Blackjack table layouts are similar at every casino, but it is essential to know where things go. An area above is where the dealer’s cards go, and the areas below are for each player’s cards and bets. Take a look at the following blackjack table chart to understand the layout for this type of game entirely:
Flash scores football live scores have all the latest football scores, fixtures and accurate football Add bets like in real bookmakers and compete with other users Livecore.cz – website for soccer fans! Here you can find games that are being played today, as well as all major league game scores from around the world! 2.6M views|original sound – LiveScore soccer livescore – the 1st live score service on the internet, powered by livescore.com, no.1 ranked soccer website. over 1000 live soccer games weekly, from every corner of the world. ผลบอลล่าสุด | ผลฟุตบอลพร้อมราคาบอล | เปรียบเทียบราคาบอล | สรุปผลบอล | ตารางแข่งฟุตบอลทุกลีก
https://www.heritageplantationgolfcourse.com/community/profile/molly8714903735/
Which countries stand between England and a place in their first World Cup final for 56 years? And which other giants of international football could meet in Qatar? © 2022 777score.com Founded in 1998 and registered in Gibraltar, LiveScore has become one of the most popular apps for fans to keep up-to-date with scores from leagues around the world. REFRESH Flashscore.mobi provides live football scores – mobile livescore. This mobile version has different parameters than Flashscore.com website for technical reasons. Soccer live scores and results are offered from all soccer leagues in the world: While we cover the top leagues from all over the world, we take a special focus on Brazilian football, competitions and results of matches in the country. The list of the presented events includes competitions of both the world’s largest tournaments and minor national leagues. You can view the fixtures not only for today but also for the coming days, as well as the results of any sporting event in the live mode.
Hey very cool web site!! Guy .. Excellent .. Wonderful ..
I’ll bookmark your site and take the feeds additionally?
I’m glad to find numerous useful info here in the publish,
we need work out more strategies on this regard, thank you for sharing.
. . . . .
Gnrh analogs act directly to start your progress with your fallopian tube disease, ls19 6ba cheap generic cialis
zithromax purchase Lenzi E, Henriksen Lacey M, Molina B, Langer J, de Albuquerque CDL, Jimenez de Aberasturi D, Liz MarzГЎn LM
Its like you read my mind! You appear to know so much about this, like you wrote
the book in it or something. I think that you can do with a few pics to drive the message home a little bit, but instead of
that, this is magnificent blog. A fantastic read.
I’ll certainly be back.
Really when someone doesn’t know then its up to other users that they will help, so here it happens.
Hey, wait, wait, don’t skip; I know you write every blog post
so well. Keep up the good work, and best of luck! And I know a good platform that can help you make $300 by just clicking ads.
I know you won’t believe me, which is why I want you to
sign up from this link and figure everything by yourself: tech-vedant.blogspot.com.
buy cialis online without a prescription Essentially, bradykinin induced angioedema involves the generation of an auto amplification circuit
Common side effects people have besides Dehydration cialis generic reviews The prognosis of patients with tubular carcinoma was excellent Table III, Figure 1
Hello! I simply would like to give you a huge thumbs up for the excellent information you’ve got right here on this post.
I am coming back to your blog for more soon.
Hi! I’m at work surfing around your blog from my new iphone 3gs!
Just wanted to say I love reading your blog and
look forward to all your posts! Keep up the great
work!
Hi are using WordPress for your site platform?
I’m new to the blog world but I’m trying to get started and create my own. Do you require any
html coding knowledge to make your own blog?
Any help would be greatly appreciated!
Hi! I know this is kind of off topic but I was wondering
if you knew where I could get a captcha plugin for my comment form?
I’m using the same blog platform as yours and I’m having difficulty finding one?
Thanks a lot!
generic cialis Here we provide an evidence suggesting that breast cancers require PAK1 for their estrogen dependent growth
hi!,I really like your writing very so much! proportion we keep in touch
more approximately your post on AOL? I need an expert
on this area to resolve my problem. Maybe that’s you!
Having a look ahead to look you.
Piece of writing writing is also a fun, if you be acquainted with
then you can write or else it is complex to write.
Wonderful article! This iss the kind of info that are meant to be
shared accross the net. Disgrace on the search
engines for not positioning this post upper! Come on over and visiit my ssite
. Thanks =)
It’s remarkable to go to see this web page and reading the views of all mates concerning this post, while I am also zealous
of getting knowledge.
Link exchange is nothing else but it is simply placing
the other person’s blog link on your page at suitable place and other person will
also do same for you.
Thank you for some other excellent article. Where else may just
anybody get that kind of info in such an ideal
approach of writing? I have a presentation subsequent week, and I am on the look for
such information.
When someone writes an piece of writing he/she retains the thought of a
user in his/her mind that how a user can understand it. So that’s
why this piece of writing is great. Thanks!
Hmm it looks like your website ate my first comment (it was super long) so I guess I’ll just sum it up what I submitted
and say, I’m thoroughly enjoying your blog. I too am an aspiring blog writer but I’m still new to everything.
Do you have any points for rookie blog writers?
I’d genuinely appreciate it.
I know this if off topic but I’m looking into starting my
own blog and was wondering what all is required to get set up?
I’m assuming having a blog like yours would cost a pretty penny?
I’m not very internet smart so I’m not 100% positive. Any suggestions or advice would be greatly appreciated.
Kudos
This piece of writing is in fact a fastidious one
it helps new the web visitors, who are wishing in favor of blogging.
Thanks for sharing your thoughts about site. Regards
I think that everything said was very reasonable. However,
what about this? suppose you typed a catchier post
title? I am not saying your information is not good, but suppose you added a title to possibly grab folk’s attention? I
mean Retroverted Uterus During Pregnancy: Causes, Symptoms &
Diagnosis! is a little boring. You ought to look
at Yahoo’s front page and watch how they create article titles
to get people to open the links. You might try adding a video or a related pic or two to get readers interested about everything’ve written. In my opinion, it could make your blog a little
livelier.
Interestingly, we observed the highest density of Gdf11 expression in the habenula and our results align with a recent habenula focused single cell RNA sequencing paper which reported Gdf11 within the top 25 of highly expressed genes in the region 25 buying priligy online Be careful and be sure to specify the information on the section Special warnings and precautions for use in the instructions to the drug Tamoxifen HEXAL directly from the package or from the pharmacist at the pharmacy
Game slot online ialah salah satu permainan yang ada dalam situs judi online yang populer di kalangan masyarakat Indonesia. Apalagi situs judi slot online terpercaya yang menggunakan sistem fair play dalam permainannya. Dari sekian banyak bandar slot online yang bertebaran di Indonesia, hanya beberapa saja yang memiliki sertifikat resmi di bawah Lembaga Perjudian Internasional. Populernya permainan judi slot online ini apalagi sejak pandemi melanda, namun anda harus tetap berhati-hati dalam memilih situs judi slot online di Indonesia. Book of Dead adalah slot video yang berjalan di platform perangkat lunak Play’n GO. Slot ini memiliki 5 gulungan dan 10 paylines, dan ini terinspirasi dengan Mesir Kuno, dan budaya mereka. Gim ini mengikuti penjelajah Rich Wild dan petualangannya. Slot ini memiliki desain yang luar biasa dengan 5 gulungan cokelat yang dipasang pada bingkai hiasan emas. Pemain dipersilakan untuk mencoba permainan ini di sini untuk bersenang-senang, atau mengunjungi Kasino Play’n GO mana pun untuk bermain secara nyata.
https://milkyway.cs.rpi.edu/milkyway/show_user.php?userid=3805322
Dice Dreams Free Rolls – Collect Daily Gifts and Rewards :-If you’re a fan of dice games, you’ll … Dice Dreams Free Rolls – Collect Daily Gifts and Rewards :-If you’re a fan of dice games, you’ll … An email with the subject line “You just got a gift card from (sender’s name)” will be sent to the recipient email address. All is left is to follow the instructions within the email. Please note that you cannot redeem or cash out your Playtika Rewards Status Points in any way. Only Reward Credits may be redeemed, as described in the CR Rules above. Status Points have no cash value. Status Points and Reward Credits are specific to each account and are not transferable to any other account. An email with the subject line “You just got a gift card from (sender’s name)” will be sent to the recipient email address. All is left is to follow the instructions within the email.
Good day! I simply wish to offer you a big thumbs up forthe great information you have right here on this post. I’ll becoming back to your blog for more soon.
Soccer livescore service, Soccer live scores and results, cups and tournaments information – all at HongKongScore.com MORE: How the USA can qualify for the 2022 World Cup in Qatar © 2023 777score.co.uk © 2023 777score.co.uk Get started UEFA Nations League 03-1 11:50 -> 1.62 – 2) Over 1.5 : Over 1.5 Goals tips. Competition Previews Puoi vedere la versione Italian su BeSoccer.com. Midfielders: Philippe Coutinho, Emiliano Buendía, Douglas Luiz, Boubacar Kamara, Leander Dendoncker, John McGinn, Jacob Ramsey, Marvelous Nakamba, Morgan Sanson There are only three matches left in CONCACAF regional World Cup qualifying and the picture is growing pretty clear. Only the top three earn automatic berths to the 2022 World Cup, while fourth-place advances to a play-in match against a team from Oceania.
https://beckettdoua008929.ageeksblog.com/19652916/football-results-live
Keep across all the football you can watch on Sky Sports with action from the Scottish Premiership, as well as Championship matches on Boxing Day. REFRESH There is no data available at this time. Please check back soon. Livecore.cz – website for soccer fans! Here you can find games that are being played today, as well as all major league game scores from around the world! Wednesday, 04 January Customize our Free Livescores Widget and use it in your website. Our app is now available on Google Play. Deptford’s own Black Horse is committed to screening Premier League and international football matches from a projector. Pair the sporting action with a pizza from the pub’s own ‘Sourdough Saloon’. For information regarding advertising, employment, results or general enquiries please Contact Us
ЛОВЕЧ – 99-33-39 Розовый кварц эффективно улучшает кровообращение, обеспечивает укрепление мышц и повышение их эластичности. Sestdiena: Brīvs Добрый день, Инна, благодарим Вас за покупку и отзыв. Действительно, в комплексе ролик работает намного лучше и эффект при длительном применении будет более заметен. Желаем самых лучших результатов. -Кварцовий ролик Хотите купить ролик Россмана, но не знаете, как им пользоваться? Смотрите нашу статью о том, как массировать лицо с помощью ролика. Нанесите ежедневное увлажняющее средство (сыворотка, крем, маска) на очищенную кожу лица, после чего обработайте лицо массажными роликами. Не превышайте работу массажером более 5-10 минут за один раз.
https://atomic-wiki.win/index.php?title=Белый_воск_для_бровей
Stylist Color Pro — это блестящий салонный уровень окрашивания в домашних условиях! ТД АзимутТрейд компания по продаже сырья для производства полимерных изделий (специализация: купить азофоску, купить едкий… Отзывы о Kerastase Маска Resistance Extentioniste для усиления прочности волос в процессе их роста 8 (499) 734-17-59 Сильное средство против старения. Стимулирует обновление клеток. Увлажняет кожу, обеспечивая эластичность. Легкая эмульсия. Отзывы о ChocoLatte Масло-бальзам для волос ФОРМУЛА №3 для сухих ломких и поврежденных волос Приобрела для мамы Нано Ботокс, и не столько для лица, сколько для области шеи и декольте, ведь именно эти зоны выдают истинный возраст женщины. Конечно, мама использует эту сыворотку и для лица тоже, но реже, т.к. кожа лица у неё была более гладкая. Ну, а теперь, благодаря Нано Ботокс, и шея, и грудь стали «соответствовать» гладкому лицу. Сыворотка реально работает!
And the people will insist on turning out in all squares, senior Muslim Brotherhood official Farid Ismail said viagra priligy
User-Friendly Interface: One of the standout features of CandyMail.org is its user-friendly interface. The platform is designed to be intuitive and easy to navigate, ensuring that users can seamlessly send and receive emails without any technical expertise. Whether you are a tech-savvy individual or a beginner, CandyMail.org caters to users of all levels of proficiency.
Yes. We offer both play and real money tables on our mobile site. After you choose your game, you can change the play mode to “Real Money” or “Play Money”. No matter if you’re at a bar, at the beach or waiting for your bus, you’ll find plenty of options to play some authentic poker right on your Android device. There are plenty of online poker sites and dedicated apps kitted out so that you can easily enjoy a great hand on the move. Get ready to play against real players with real money. Playing an Android poker app for real money couldn’t be simpler. All you need is a mobile device with an Android operating system and a good internet connection. Simply find the mobile online version of poker for Android you wish to play at an online poker room. There will be versions for most operating systems, including Android, on most sites.
https://magic-wiki.win/index.php?title=Best_sports_gambling_sites_canada
Playstar adalah pengembang game slot online yang berkantor pusat di Asia dan telah lama beroperasi di pasar Asia dan Amerika. Slot Playstar menyediakan jenis game slot dengan tema yang beragam, mencakup slot oriental, slot bertema petualangan, dan slot bertema laut. Beberapa slot Playstar yang wajib dimainkan yaitu Fu Lu Shou, Dragon King, dan Mystery Lake of Pearl. Masih mencari kumpulan daftar situs judi slot online terpercaya yang fair play? Sekian banyak bandar slot online yang bertebaran di internet pasti membuat anda bingung, mana situs judi slot online bonafit dan mana yang tidak bonafit bagi para pemain. Permainan slot online sangat populer dan disukai oleh kalangan masyarakat Indonesia terutama di kota-kota besar. Apalagi saat menghadapi pandemi yang tak kunjung habis ini, orang – orang berbondong-bondong mencari situs judi slot online terpercaya 2022 untuk mengisi waktu luangnya.
purchase cialis online cheap fortuitum are, although both of these mycobacteria are often susceptible to fluoroquinolones, gentamicin, and doxycycline
Thank you for any other wonderful article. Where else may anyone get that kind of information in such a perfect method of writing? I have a presentation next week, and I am at the look for such information.
Эта статья – источник вдохновения и новых знаний! Я оцениваю уникальный подход автора и его способность представить информацию в увлекательной форме. Это действительно захватывающее чтение!
how long does it take viagra to work My OB- GYN prescribed clomid without an HSG, but when I switched to the best fertility clinic in the Southeast, they required an HSG before any meds were given
Thanks for finally writing about >Retroverted Uterus During Pregnancy: Causes, Symptoms &
Diagnosis! <Liked it!
whoah this weblog is fantastic i really like reading your posts.
Keep up the good work! You recognize, a lot of persons are hunting
round for this info, you can help them greatly.
My family members all the time say that I am wasting my time
here at web, however I know I am getting familiarity everyday by reading
such fastidious articles.
Приемник ЛИРА РП-248-1 основан на супергетеродинном принципе и имеет шесть диапазонов частот, которые позволяют принимать радиосигналы в диапазоне от 0,15 до 30 МГц. Приемник имеет возможность работы в различных режимах, включая АМ, ЧМ, СВ и ДСВ.
Есть абсолютно бесплатная доска объявлений. Очень простая. Минимум модерации. Можно ставить ссылки прямо в тексте. доска объявлений
Hi would you mind sharing which blog platform you’re using?
I’m planning to start my own blog in the near future but
I’m having a tough time selecting between BlogEngine/Wordpress/B2evolution and
Drupal. The reason I ask is because your layout seems different then most
blogs and I’m looking for something completely unique.
P.S Apologies for getting off-topic but I had to ask!
Download our award-winning and secure software Otro lugar famoso : el casino de Tarragona, que se puede encontrar cerca del anfiteatro romano de la ciudad. Con su elegante decoración, este establecimiento da la bienvenida a muchos visitantes que vienen a disfrutar de máquinas tragaperras, mesas de juego y póker. Gracias a un enorme patrimonio cultural e histórico, España es un destino popular para los turistas. Hogar de la familia real, este centro económico está llena de monumentos, museos, galerías de arte, así como los centros comerciales, tiendas de moda y lugares de entretenimiento. El Palacio Real, el Museo del Prado, el barrio de Chueca, el parque de Retiro o los asientos del estadio Santiago Barnabeu son importantes.
https://wiki-velo.win/index.php?title=Juegos_de_tragamonedas_para_jugar_gratis_sin_descargar
No solo podrás divertirte con la Ruleta Online, sino que gracias a nuestras promociones de bienvenida podrás sacarle también el máximo partido. En iJuego contamos con las promociones más atractivas y con diferentes bonos para que, incluso, puedas jugar en un primer momento sin gastar dinero. Una vez que ya hayas practicado, basta con registrarse para empezar a apostar y beneficiarte de nuestros premios. ¡No dudes en darle a esta Ruleta de Casino Online una gran oportunidad! ¿Preparado para un buen rato de acción en nuestro casino en vivo? Lo único que tendrás que hacer para jugar en el casino en vivo de JOKERBET será entrar en la nueva sección de casino en vivo y elegir alguna de las ruletas que ponemos a tu disposición. Podrás acceder desde todos los dispositivos, estés donde estés y a cualquier hora.
https://www.charlie-levy.com/
But in the event of a relapse, and especially a second relapse, spouses should at least consider getting tested cialis prices Group 4 SAD VGX indomethacin n 6; rats with SAD VGX pretreated with 10 mg kg indomethacin IV administered 10 minutes before the first intravenous metformin injection
Los Juegos Infantiles Pum son hablados en español, para jugar gratis y online, destinados a bebés, niñas y niños a partir de 1 año, y con propuestas para nenes y nenas de 2, 3, 4 y 5 años aproximadamente. En la categoría Arcade de Google Play encontramos divertidos e imprescindibles juegos sin conexión como Crossy Road,Angry Birds y Fruit Ninja, o a juegos recientes como Pureya, entre otros. ¡Todos los días son una oportunidad para que los más pequeños aprendan algo nuevo con Triviatopia! Al presentar la capacidad de ejecutarse sin conexión a Internet ni WiFi, te recomendamos esta opción de juego de acción en tercera persona, en el cual los jugadores tienen que controlar a uno de los pocos sobrevivientes a un cataclismo global y así, enfrentarse a las criaturas del apocalipsis. Teniendo presente que, el sistema de control de la app es muy tradicional porque cuenta con botones para mover hacia la izquierda o derecha con el fin de esquivar y también para hacer golpes especiales. Sin embargo, no es una app del todo ideal porque debe descargarse únicamente en dispositivos que posean a partir de 1 GB y solo podrás jugar los primeros seis niveles gratuitamente.
http://dyland.co.kr/board/bbs/board.php?bo_table=free&wr_id=1568901
Home kinkykarma.co.uk groups online-casino-mit-paypal-1-euro-einzahlung-online-casino-mit-paypal Por lo general, no. Jugar gratis implica que no hay ningún tipo de transacción económica entre el casino y el usuario, y el juego instantáneo y sin registro contribuye a esto. Algunos casinos ofrecen bonos sin depósito, pero para poder retirarlos aún deberás apostar dinero real. Tu dirección de correo electrónico no será publicada. Los campos obligatorios están marcados con * Bingo Clash está disponible para mayores de 17 años. Se puede descargar en forma gratuita desde la App Store de Apple. El juego consta de un diseño de 5 carretes y 5 filas con 50 líneas de pago fijas, metodo para ganar ala ruleta algunos de nuestros casinos en línea favoritos están a cargo de casino Group. La jugabilidad se acompaña de música al estilo Indiana Jones que sirve para crear un aura de misterio y aventura, pero la experiencia general hace que sea fácil recomendar el video póquer a cualquiera que esté buscando disfrutar de la acción del juego mientras viaja. Por lo tanto, existen límites de retiro establecidos. Verás que te hemos proporcionado acceso con un solo clic para que llegues a nuestras marcas aprobadas, aunque.
Your style is very unique compared to other folks I’ve read stuff from.
I appreciate you for posting when you have the opportunity, Guess I will just book mark
this page.
Hmm it appears like your blog ate my first comment (it was extremely long) so I guess I’ll just
sum it up what I wrote and say, I’m thoroughly enjoying
your blog. I as well am an aspiring blog writer but I’m still new to everything.
Do you have any suggestions for inexperienced
blog writers? I’d certainly appreciate it.
Hey there! I could have sworn I’ve been to this site before but after browsing through some of the post I
realized it’s new to me. Nonetheless, I’m definitely happy
I found it and I’ll be bookmarking and checking back often!
Norweski pokerzysta zwyciężył w turnieju #21-H: NLHE 6-Max Progressive KO (harmonogram tutaj). Wpisowe w wysokości 5.200$ opłacono 108 razy, a Preben otrzymał 140.110$. To drugi tytuł WCOOP w karierze Norwega. Trzy lata temu wygrał turniej #65: NLHE Progressive KO za 2.100$ (160.824$). Norweski pokerzysta zwyciężył w turnieju #21-H: NLHE 6-Max Progressive KO (harmonogram tutaj). Wpisowe w wysokości 5.200$ opłacono 108 razy, a Preben otrzymał 140.110$. To drugi tytuł WCOOP w karierze Norwega. Trzy lata temu wygrał turniej #65: NLHE Progressive KO za 2.100$ (160.824$). Na PokerStars trwa festiwal World Championship of Online Poker. Wśród zawodników, którzy mogą pochwalić się tytułem, jest Preben „prebz” Stokkan. Na PokerStars trwa festiwal World Championship of Online Poker. Wśród zawodników, którzy mogą pochwalić się tytułem, jest Preben „prebz” Stokkan.
http://goodbuilder.bokslee.com/bbs/board.php?bo_table=free&wr_id=2465
Poker w STS to bukmacherska odmiana najpopularniejszego pokera na świecie, czyli Texas Hold’em. Gracz stawia czy jego układ pokona karty krupiera. W zakładach wystawione są kursy podobnie jak w przypadku wydarzeń sportowych, a więc nie gramy bezpośrednio na pieniądze, a jedynie obstawiamy zwycięstwo. Poker online za darmo i bez rejestracji dostępny jest na naszej stronie. Legalną możliwość zagrania za darmo w demonstracyjną wersję pokera online posiada również na swojej stronie Total Casino. Legalny poker online – gdzie zagrać w pokera przez internet? Rozgrywki pokerowe u bukmacherów. Gra w pokera przez internet nie wymaga od nas niczego szczególnego, poza znajomością zasad rozgrywki i – rzecz jasna – dostępu do internetu. Obecnie możemy sprawdzać swoje umiejętności w wielu odmianach pokera, w tym najpopularniejszym Texas Hold’em, nie tylko w komputerze, ale także w smartfonie czy tablecie i to nawet będąc poza domem – w tramwaju, autobusie czy na biwaku pod namiotem.
priligy united states Another interesting question is whether subcutaneous fibrosis can be prevented, or at least reduced
Diabetes mellitus and the metabolic syndrome where can i order levitra
no credit card dating sites: new singles online – pof dating sites usa
generic prednisone otc: https://prednisone1st.store/# where to get prednisone
If some one desires to be updated with hottest technologies therefore he must be pay a visit
this website and be up to date daily.
bob cialis commercial best tadalafil brand in india cialis reviews by users
Разрешение на строительство — это официальный удостоверение, предоставленный правомочными органами государственной власти или местного руководства, который дает возможность начать строительство или осуществление строительных операций.
Разрешение на строительство недвижимого имущества задает правовые принципы и регламенты к стройке, включая дозволенные категории работ, приемлемые материалы и методы, а также включает строительные нормы и пакеты охраны. Получение разрешения на строительство является обязательным документов для строительной сферы.
I’ve been exploring for a bit for any high-quality articles or
weblog posts on this kind of space . Exploring in Yahoo I finally stumbled upon this website.
Reading this information So i’m happy to express that I have a very just right uncanny feeling I
found out just what I needed. I such a lot
certainly will make sure to don?t disregard this web site and give it
a look on a continuing basis.
Wow, superb blog layout! How long have you been blogging for?
you make blogging look easy. The overall look of
your website is fantastic, as well as the content!
Быстровозводимые здания – это прогрессивные строения, которые отличаются громадной скоростью возведения и мобильностью. Они представляют собой сооружения, образующиеся из эскизно созданных элементов или модулей, которые имеют возможность быть быстрыми темпами установлены в месте стройки.
[url=https://bystrovozvodimye-zdanija.ru/]Строительство помещений из сэндвич панелей[/url] владеют гибкостью и адаптируемостью, что дает возможность просто изменять а также переделывать их в соответствии с интересами покупателя. Это экономически успешное а также экологически устойчивое решение, которое в последние лета приобрело широкое распространение.
This page really has all of the information I needed about
this subject and didn’t know who to ask.
[url=https://forfreedating.co.uk/]Our dating platform[/url] is the perfect way to meet interesting people who are searching for love.
Our web-based platform enables you to connect with compatible partners anytime, anywhere.
Become a part of our online community today and start your journey to finding love with Flirt finder.
Join [url=https://freeflir-online.com/]Flirt Finder[/url] and find the digital romance.
Hi there friends, pleasant article and nice urging commented
here, I am truly enjoying by these.
El mejor exchange para invertir en bitcoin (o en otros pares de criptomonedas) es aquel que funciona a la perfección, que da toda la información necesaria o que tiene un proceso de registro sencillo y fácil. Además, Material Bitcoin no solo vende wallets, sino que cuenta con una plataforma que permite la compra directa de Bitcoin a través de su web. Para realizar esto, cuenta con la regulación del Banco de España, pues está inscrita en el Registro de proveedores de servicios de cambio de moneda virtual por moneda fiduciaria del con el número D701. Pero no todos los exchanges son iguales. Algunos ofrecen más variedad de criptomonedas, otros tienen mejores comisiones, otros son más fáciles de usar y otros tienen más seguridad y reputación. Por eso, es importante elegir bien el exchange que mejor se adapte a nuestras necesidades y expectativas. En este artículo, te vamos a presentar los mejores exchanges de criptomonedas de 2023 según nuestro criterio y experiencia.
https://elliottconk174179.thezenweb.com/analizar-criptomonedas-57969394
Početna stranica Objavljeno: 24.07.2023 | Autor: Ivan Horvatić Live Bitcoin price (BTC) including charts, trades and more. Create real-time notifications and alerts to follow any changes in the Bitcoin value. Que Es Bitcoin Cash BCH 2023 | Es el Bitcoin Real? | Bitcoin vs Bitcoin Cash binarna opcija paxforex Hatta Timur, geçen sezon görüşüp de alamadığı isimler arasında en çok Alexis’in içinde ukde olarak kaldığını açıklamıştı. Taraflar önümüzdeki günlerde tekrar yemekte buluşacak. Transfer gerçekleşirse Sanchez, 1 yıl gecikmeli olarak Galatasaray’a imza atacak. Izvor: BING Bonservisi elinde olan 34 yaşındaki Şilili futbolcuyla Sportif A.Ş Başkanvekili Erden Timur bir görüşme gerçekleştirdi. 1.69 boyundaki futbolcunun sarı-kırmızılı ekibe yeşil ışık yaktığı öğrenildi.
Моментально возводимые здания: экономический доход в каждой детали!
В современной действительности, где секунды – доллары, здания с высокой скоростью строительства стали реальным спасением для коммерческой деятельности. Эти современные конструкции включают в себя высокую надежность, финансовую экономию и мгновенную сборку, что сделало их первоклассным вариантом для разных коммерческих начинаний.
[url=https://bystrovozvodimye-zdanija-moskva.ru/]Стоимость быстровозводимого здания под ключ цены[/url]
1. Ускоренная установка: Часы – ключевой момент в бизнесе, и скоро возводимые строения способствуют значительному сокращению сроков возведения. Это значительно ценится в сценариях, когда актуально оперативно начать предпринимательство и начать получать доход.
2. Экономия средств: За счет совершенствования производственных процессов элементов и сборки на площадке, расходы на скоростройки часто уменьшается, по сопоставлению с обыденными строительными проектами. Это позволяет сократить затраты и достичь более высокой инвестиционной доходности.
Подробнее на [url=https://xn--73-6kchjy.xn--p1ai/]http://scholding.ru/[/url]
В заключение, объекты быстрого возвода – это превосходное решение для бизнес-мероприятий. Они объединяют в себе скорость строительства, финансовую выгоду и надежность, что обуславливает их оптимальным решением для предпринимателей, ориентированных на оперативный бизнес-старт и получать деньги. Не упустите момент экономии времени и средств, оптимальные моментальные сооружения для вашего предстоящего предприятия!
Быстромонтажные здания: финансовая польза в каждой составляющей!
В сегодняшнем обществе, где время имеет значение, скоростройки стали настоящим выходом для бизнеса. Эти новаторские строения объединяют в себе высокую прочность, эффективное расходование средств и молниеносную установку, что обуславливает их идеальным выбором для различных коммерческих проектов.
[url=https://bystrovozvodimye-zdanija-moskva.ru/]Легковозводимые здания из металлоконструкций[/url]
1. Молниеносное строительство: Секунды – самое ценное в экономике, и экспресс-сооружения обеспечивают существенное уменьшение сроков стройки. Это преимущественно важно в постановках, когда срочно нужно начать бизнес и начать извлекать прибыль.
2. Экономия средств: За счет улучшения процессов изготовления элементов и сборки на объекте, расходы на скоростройки часто оказывается ниже, по сравнению с обычными строительными задачами. Это позволяет сократить затраты и получить более высокую рентабельность инвестиций.
Подробнее на [url=https://xn--73-6kchjy.xn--p1ai/]https://scholding.ru[/url]
В заключение, скоростроительные сооружения – это оптимальное решение для коммерческих инициатив. Они включают в себя быстрое строительство, экономическую эффективность и устойчивость, что обуславливает их превосходным выбором для предприятий, ориентированных на оперативный бизнес-старт и выручать прибыль. Не упустите момент экономии времени и средств, выбрав быстровозводимые здания для вашего следующего делового мероприятия!
Understanding Flirt Finders: What Are They?
Flirt finder dating sites are a specialized niche in the world of online dating. They cater to individuals who are looking for more than just a simple chat or a plain swipe right. These platforms are designed to help people find meaningful connections, whether they’re seeking a committed relationship or a exciting romance. The emphasis here is on the art of flirting, building chemistry, and creating sparks between potential partners.
The Allure of Flirt Finders
A Lively Twist on Dating
One of the spellbinding aspects of [url=https://flklined2s.nl/]flirt finder[/url] is their cheerful approach to dating. Unlike standard dating platforms that primarily focus on profiles and images, flirt finders encourage users to partake in flirty conversations and clever banter. This approach creates an exhilarating and flirtatious ambiance, transforming each interaction into what feels like a potential escapade.
A Multifaceted Community
Flirt finder dating sites frequently boast a wide-ranging user base, simplifying the quest for someone who aligns with your desires. Whether you’re in search of a companion with particular passions or a partner with a specific way of life, these platforms offer an array of potential matches to explore.
Enhanced Communication Tools
Effective communication is essential in any successful relationship. Flirt finder sites provide a variety of instruments such as video chats, virtual presents, and interactive games that facilitate connecting with others. These capabilities go above and beyond simple text messages and support users in expressing themselves in creative ways.
Compatibility Matching
Many flirt finder dating sites employ sophisticated algorithms to match users based on suitability factors. These algorithms take into account interests, values, and personality traits, heightening the likelihood of uncovering a significant connection.
Crafting an Unforgettable Profile
Your profile is your digital first impression on a flirt finder site. To distinguish yourself, utilize high-quality photos that display your personality, and compose a engaging bio that spotlights your interests and what you’re looking for in a partner. Bear in mind, authenticity is essential.
Etiquette for Flirting
Flirting on these platforms is completely about being appealing and respectful. Certainly, join amusing banter and compliment your potential matches, but steer clear of exceeding boundaries or making anyone appear uncomfortable. Respect forms the essence of any productive interaction.
Site: [url=https://flklined2s.nl/]www.flklined2s.nl[/url]
Discovering Exciting Features
Take advantage of the distinctive features provided by flirt finder sites. Transmit virtual gifts, engage in icebreaker games, and make use of video chats to get to know your potential matches better. These tools can assist you in breaking the ice and creating unforgettable connections.
Why Opt for a Flirt Finder Dating Platform?
Revitalize Your Love Journey
If your love life desires an increased dose of excitement, flirt finder dating platforms are the ultimate remedy. They provide a rejuvenating respite from the tedium of traditional dating and infuse a notion of playfulness into the journey.
Unearth Kindred Spirits
These platforms attract individuals who emulate your enthusiasm for flirting and building romantic bonds. This shared common ground can lead to deeper and satisfying interactions.
Elevated Chances of Success
The emphasis on harmony and significant connections on flirt finder platforms frequently brings about elevated success rates when it comes to unearthing compatible partners. If you’re genuinely devoted to seeking love, these platforms have the potential to be a turning point.
Conclusion
Flirt finder dating sites have changed the way we approach dating. Their lighthearted style, variety of users, and cutting-edge tools offer a unique and exciting path to unearth love or a deep connection.
So, if you’re prepared to enhance your dating life and embark on the world of flirting, give flirt finder dating sites a chance.
Your forthcoming thrilling adventure in love could be just a click away.
Прогон сайта с использованием программы “Хрумер” – это способ автоматизированного продвижения ресурса в поисковых системах. Этот софт позволяет оптимизировать сайт с точки зрения SEO, повышая его видимость и рейтинг в выдаче поисковых систем.
Хрумер способен выполнять множество задач, таких как автоматическое размещение комментариев, создание форумных постов, а также генерацию большого количества обратных ссылок. Эти методы могут привести к быстрому увеличению посещаемости сайта, однако их надо использовать осторожно, так как неправильное применение может привести к санкциям со стороны поисковых систем.
[url=https://kwork.ru/links/29580348/ssylochniy-progon-khrummer-xrumer-do-60-k-ssylok]Прогон сайта[/url] “Хрумером” требует навыков и знаний в области SEO. Важно помнить, что качество контента и органичность ссылок играют важную роль в ранжировании. Применение Хрумера должно быть частью комплексной стратегии продвижения, а не единственным методом.
Важно также следить за изменениями в алгоритмах поисковых систем, чтобы адаптировать свою стратегию к новым требованиям. В итоге, прогон сайта “Хрумером” может быть полезным инструментом для SEO, но его использование должно быть осмотрительным и в соответствии с лучшими практиками.
Добро пожаловать в нашем сайте, вашего надежного партнера в мире [url=https://texttospeech.ru/]спортивные прогнозы бесплатно[/url]. Мы с гордостью предоставляем вам шанс взять на себя контроль над вашими ставками и увеличить свои шансы на успех. Наши профессиональные аналитики и специалисты следят за событиями в мире спорта, чтобы обеспечить вас свежими и точными советами.
Почему выбирать нас:
Экспертные прогнозы: Наши специалисты работают не покладая рук, чтобы предоставлять вам прогнозы на все популярные виды спорта. Мы знаем, насколько важно получать качественные советы перед тем, как сделать ставку.
Широкий выбор: Мы предлагаем ставки на разнообразные виды спорта, включая футбол, баскет, теннис, мяч и многое другое. Вы можете отбирать из множества событий и наслаждаться страсть на свой вкус.
Бесплатные прогнозы: Мы верим, что каждый может получить доступ к полезным советам. Поэтому мы предлагаем бесплатные советы, чтобы поддержать вас сделать успешные ставки.
Простота и удобство: Наш веб-сайт и приложение для мобильных устройств разработаны с учетом вашего удовольствия. Сделайте ставку всего в несколько кликов.
Как начать:
Зарегистрируйтесь: Создайте свой аккаунт в нашем ресурсе и получите доступ к нашему полному спектру услуг.
Получайте предсказания: Подписывайтесь на бесплатные советы и получайте свежие советы от наших экспертов.
Сделайте ставку: После того как вы получили полезный совет, сделайте ставку на команду по душе или событие и получайте удовольствие от игры.
Вознаграждение за успех: Вместе с нашим ресурсом, вы имеете возможность к вашей победе. Попробуйте нашу помощь уже сегодня и погружайтесь в мир ставок на спорт во всей его красе!
Добро пожаловать в texttospeech.ru, вашего проверенного союзника в мире [url=https://texttospeech.ru/]спортивные прогнозы[/url]. Мы с гордостью предоставляем вам шанс взять на себя контроль над вашими ставками и увеличить свои перспективы на успех. Наши опытные эксперты и эксперты следят за событиями в мире спорта, чтобы обеспечить вас актуальными и точными советами.
Почему выбирать нас:
Качественные аналитические прогнозы: Наши специалисты усердно трудятся, чтобы предоставлять вам предсказания на все популярные виды спорта. Мы знаем, как важно получать качественные советы перед тем, как сделать ставку.
Широкий выбор: Мы предлагаем ставки на разнообразные виды спорта, включая футбол, баскетбол, ракетку, мяч и многое другое. Вы можете выбирать из множества событий и наслаждаться азарт на свой вкус.
Советы без оплаты: Мы верим, что каждый должен иметь доступ к качественным прогнозам. Поэтому мы предлагаем бесплатные предсказания, чтобы поддержать вас сделать успешные ставки.
Простота и удобство: Наш веб-сайт и приложение для мобильных устройств разработаны с учетом вашего комфорта. Сделайте ставку всего в несколько кликов.
Как начать:
Создайте аккаунт: Создайте персональный профиль в нашем ресурсе и получите доступ к всем нашим сервисам.
Получайте прогнозы: Подписывайтесь на наши бесплатные прогнозы и получайте свежие советы от наших экспертов.
Поставьте свою ставку: После того как вы получили свой прогноз, сделайте ставку на команду по душе или событие и получайте удовольствие от игры.
Вознаграждение за успех: Вместе с texttospeech.ru, вы владеете ключами к вашей победе. Попробуйте наши услуги уже сегодня и переживайте в мир ставок на спорт во всей его красе!
I’m curious to find out what blog system you happen to be using?
I’m experiencing some small security issues with my latest
blog and I would like to find something more safe.
Do you have any recommendations?
Покрытие пола – существенный шаг при ремонте. Укладка пола позволяет добиться ровную основу для финишной облицовки.
Мастера осуществляют [url=https://styazhka-pola24.ru/]стяжка пола под ключ[/url] с учетом всех норм и стандартов. Выравнивание пола осуществляется с применением современных компонентов, которые обеспечивают надежное покрытие и стойкость.
Устройство пола даёт возможность сформировать идеальное основание для разнообразных видов облицовки. В Москве выравнивание пола выполняют опытные специалисты.
Механизированная штукатурка — новаторский подход выполнения отделки стен.
Он заключается в использовании автоматических систем штукатурки, обычно, произведенных в Германии, благодаря которым смесь подготавливается к работе и апплицируется на стену автоматически и с давлением.
[url=https://mehanizirovannaya-shtukaturka-moscow.ru/]Штукатурка стен по маякам[/url] С подтвержденной гарантией До 32 процентов выгоднее обычной, Можно клеить обои без шпаклевки от кампании mehanizirovannaya-shtukaturka-moscow.ru
В результате, повышается сцепление с поверхностью, а сроки выполнения работ сокращается в 5–6 раза, в сравнении с ручной отделкой. За счет автоматизации и упрощения рабочего процесса цена механизированной штукатурки выходит дешевле, чем при использовании традиционного подхода.
При машинном нанесении штукатурки используются специализированные смеси, стоимость которых меньше чем при ручной отделке примерно на треть. При определенных навыках специалистов, а кроме того при соблюдении всех технологических принципов, оштукатуренная поверхность получается абсолютно ровной (профессиональные стандарты) и полированной, в связи с этим последующая обработка шпатлевкой не не необходима, что обеспечивает дополнительную экономию средств заказчика.
Игра в покер – увлекательный способ провести время, как пользуется популярностью среди поклонников азарта и мастеров игры.
[url=http://alcosystems.se/wp-content/pages/1xbet_promo_codes_free.html]http://alcosystems.se/wp-content/pages/1xbet_promo_codes_free.html[/url]
[url=https://librairienumeriquemonaco.com/docs/pages/dekorativnyy_gipsokarton_opisanie.html]https://librairienumeriquemonaco.com/docs/pages/dekorativnyy_gipsokarton_opisanie.html[/url]
[url=https://hilord.com/wp-content/pages/1xbet_promo_code_free_bet_bonus_for_today.html]https://hilord.com/wp-content/pages/1xbet_promo_code_free_bet_bonus_for_today.html[/url]
[url=http://stovespareparts.ie/wp-content/pages/1xbet_promo_codes_free.html]http://stovespareparts.ie/wp-content/pages/1xbet_promo_codes_free.html[/url]
Покер предполагает различные вариации, что делает его разнообразным и интересным. Игроки могут состязаться в различных видах и получать награды.
Партейная игра в карты накладывает обязанности на участников анализа ситуации, стратегического мышления и умения читать соперников. Это придает игре особую привлекательность и увлекательной для участников разного уровня.
Партейная игра является проявлением интеллектуальных способностей и мастерства, и он предоставляет возможность завоевать значительные награды.
Группа «Каспий» родилась в конце 2012 года, в Москве, когда Володя Астапчик собрал вокруг себя группу музыкантов-единомышленников. Уже через полгода, летом 2013 года команда, названная «Каспий», дебютировала на фестивалях «Нашествие» и «Доброфест». Мелодичность, драйв и многослойная лирика текстов помогли группе стремительно завоевать Интернет- и офф-лайн аудиторию.
[url=https://kaspiymusic.ru/]группа каспий[/url]
Смешанная стяжка – метод выравнивания полов. Монтаж полусухой стяжки дает возможность получить ровное покрытие для окончательного покрытия.
[url=https://styazhka77.ru/]полусухая стяжка москва[/url] Мы сделаем супер ровную стяжку пола. 7 лет опыта работы От 500 рублей за квадратный метр
Техническое обслуживание полусухой стяжки включает в себя регулярную проверку и устранение дефектов с применением специализированных инструментов.
Специализированные инструменты для полусухой стяжки позволяет осуществить процесс устройства с высокой точностью. Частично сухая стяжка пола представляет собой эффективный вариант для обеспечения качественного основания для дальнейшей отделки.
It’s actually a nice and useful piece of information. I’m satisfied that
you shared this helpful information with us. Please stay us up to date like this.
Thanks for sharing.
I visit day-to-day some web pages and sites to read posts,
however this webpage provides quality based posts.
Thanks for your personal marvelous posting!
I quite enjoyed reading it, you happen to
be a great author.I will be sure to bookmark your blog and will come back sometime soon. I want to encourage yourself to continue your great writing, have
a nice afternoon!
Больше интересной информации о строительстве и ремонте можно прочитать на сайте [url=https://stroyka-gid.ru]https://stroyka-gid.ru[/url] .Только самые популярные статьи и обзоры процесса ремонта помещений и строительства зданий.
1хбет — востребованная букмекерская фирма. Регистрируйтесь на сайте компании и получайте бонусы. Сделайте ставку на свой фаворит. Используйте высокие шансы.
[url=https://1xbet-seychas.ru]1 xbet
Эксклюзивное объявление: мне 18 лет, и я готова подарить тебе невероятный минет в машине. Ощути магию настоящего наслаждения! [url=https://samye-luchshie-prostitutki-moskvy.top]индивидуалки тушинÑкаÑ[/url]
Интимные спутницы из Москвы готовы подарить вам незабываемые моменты. Эксклюзивное объявление: мне 18 лет, и я готова подарить тебе невероятный минет в машине. Ощути магию настоящего наслаждения! [url=https://samye-luchshie-prostitutki-moskvy.top]индивидуалки метро люблино[/url]. Профессиональные куртизанки ждут вашего звонка. Узнайте, что такое настоящее удовлетворение в компании кокеток из столицы.
Модернизация апартаментов — наша специализация. Техническое обслуживание дома в сфере жилья. Мы предлагаем восстановление квартиры с гарантированным качеством.
[url=https://remont-kvartir-brovari.kyiv.ua/]https://remont-kvartir-brovari.kyiv.ua/[/url]
[url=https://samye-luchshie-prostitutki-moskvy.top]https://samye-luchshie-prostitutki-moskvy.top[/url]
Yes! Finally someone writes about kamagra kopen telefoonnummer.
MOTOLADY предлагают услуги аренды и проката мотоциклов и скутеров в Хургаде, Эль Гуне и Сахл Хашиш. MOTOLADY – одна из самых популярных компаний по прокату мотоциклов и скутеров. Они предлагают большой выбор транспортных средств по разумным ценам. MOTOLADY компания, специализирующаяся на [url=https://motohurghada.ru/]Прокат скутера в Сахл Хашиш[/url] и Эль Гуне. Они предлагают услуги доставки транспорта в любое удобное для вас место. У нас в наличии различные модели транспортных средств по доступным ценам. Перед арендой транспорта обязательно ознакомьтесь с правилами и требованиями компании, также проверьте наличие страховки и необходимые документы для аренды.
01. Collect 1,000+ Free Chips 18+ рџЌЂ $15,000 SLOTS BONUS BUYS рџЌЂ !OFFER Share House Of Fun Free Coins with friends and checkout Pop slots free chips. Visit us daily to get Slot Machine Tournaments free spins and please recommend your friends to get 2021 bonus cards by Collect Heart of Vegas Free Coins Simply by visiting our website daily, No need to visit multiple place to find Heart of Vegas Coins, Play now on Android, iOS, PC and Facebook for Free. Free spins and bonus offers make your results worse Share Heart of Vegas Free Coins and checkout Cash Frenzy Free Coins . If you want to get the most out of your Slotpark free chips, here are some tips to keep in mind: The first casino bonus Gaminator user receives after registration, later active gamblers are awarded other rewards. The club often holds tournaments, with the opportunity to win bonuses. You can also get freespins, bonus points on a player’s birthday.
https://telegra.ph/online-casino-with-free-bonus-without-deposit-11-12
* + 250% Match Bonus and 25 Free Spins on game “Neon Wheel 7s”. Code: PEEUH (Valid Slots and Keno) The STARTER350 promo code is an intriguing option for when you make your deposit. Create and verify your new account. Make a minimum deposit, and use the coupon code STARTER350. Raging Bull Slots will match your deposit by 3.5 times, so if you deposit $20, you’ll have $20 in your cash account as well as $70 in your bonus account. There is no maximum bonus, but there are deposit limits. Raging Bull Casino is giving away 260% Bonus + … Use bonus code: VWM9MPNHH We regularly update this page with the codes posted by you, the members, in the ‘No Deposit Casinos’ section on the forum. Check back here daily for new bonuses, and while you’re here, why not help each other out? Let your fellow members know that claiming the bonus was a success, which will result in a thumbs up, and for those that were unsuccessful, you’ll see a thumbs down. You’ll also want to peruse the comments for key information regarding the codes or general comments from other members. Finally, you can spread the word to all your friends by sharing the code on your social media pages.
Эффективное изоляция наружных стен — счастье и сбережение в своем недвижимости!
Согласитесь, ваш дом заслуживает наилучшего! Тепловая изоляция облицовки – не голос решение для экономии на тепле, это вклад в благополучие и долголетие вашего здания.
? Почему тепловая изоляция с нами?
Мастерство: Наши мастера – компетентные. Мы все заботимся о каждой конкретной, чтобы обеспечить вашему домовладению идеальное утепление.
Стоимость термоизоляции: Мы все ценим ваш бюджет. [url=https://stroystandart-kirov.ru/]Утепление дома сколько стоит работа[/url] – начиная от 1350 руб./кв.м. Это вложение средств в ваше приятное будущее!
Энергосберегающие меры: Забудьте о утечках тепла! Наши материалы не только сохраняют тепловой микроклимат, но и дарят вашему коттеджу новый уровень энергоэффективности.
Создайте свой домашний уголок комфортабельным и стильным!
Подробнее на [url=https://stroystandart-kirov.ru/]http://n-dom.ru
[/url]
Не предоставляйте свой коттедж на произвольное стечение обстоятельств. Доверьтесь специалистам нашей компании и создайте уют вместе с нами-специалистами!
Оцифровка документов в архиве — это наше направление. Мы предоставляем услуги цифровизации документов с использованием современных технологий. Сотрудничество с нами — это эффективный способ сделать вашу документацию доступной в электронной форме.
Когда вопрос касается разработки своего собственного сайта, подбор хостинга играет огромное влияние – [url=https://besthost.by/virtualhosting/]хостинг сайта[/url].
Ведь именно провайдер будет влиять на доступ и быстродействие вашего сайта для посетителей. Если вы в Беларуси и хотите найти надежного поставщика услуг хостинга, то лучший выбор – это прекрасный выбор. BestHost.BY – провайдер, который имеет первенствующих компаний по хостингу в на территории Беларуси, которая предоставляет высококачественные услуги на протяжении 15 лет
[url=https://besthost.by/virtualhosting/]виртуальный хостинг[/url]
Когда речь заходит о создании своего собственного сайта, выбор хостинга играет огромную роль. Ведь именно хостинг будет определять доступность и быстродействие вашего сайта для пользователей. Если вы находитесь в Беларуси и ищете надежного хостинг-провайдера, то BestHost.BY – это отличный выбор. BestHost.BY – одна из ведущих хостинг-компаний в Беларуси, предоставляющая высококачественные услуги уже на протяжении 15 лет.
[url=https://afishkasochi.ru]1хбет[/url] – это популярная букмекерская компания, предлагающая широкий выбор ставок на спорт, казино и многое другое. С высокими коэффициентами и удобным интерфейсом, 1xbet привлекает множество игроков. Он также предоставляет возможность онлайн-трансляций событий. 1xbet создает захватывающий игровой опыт для своих пользователей.
[url=https://30palomnik.ru]1xbet рабочее зеркало[/url] – это популярная букмекерская компания, предлагающая широкий выбор ставок на спорт, казино и многое другое. С высокими коэффициентами и удобным интерфейсом, 1xbet привлекает множество игроков. Он также предоставляет возможность онлайн-трансляций событий. 1xbet создает захватывающий игровой опыт для своих пользователей.
Эффективное изоляция облицовки — комфорт и бюджетность в семейном жилище!
Согласитесь, ваш недвижимость заслуживает высококачественного! Термоизоляция облицовки – не исключительно решение для сбережения на отоплении, это вкладывание в комфорт и долгосрочность вашего здания.
? Почему тепловая изоляция с нами-мастерами?
Опыт: Наша бригада – профессионалы своего дела. Мы все заботимся о каждом элементе, чтобы обеспечить вашему домовладению идеальное утепление.
Цена изоляции: Наша бригада ценим ваш финансовые ресурсы. [url=https://stroystandart-kirov.ru/]Заказать утепление фасада[/url] – начиная от 1350 руб./кв.м. Это вложение денег в ваше удовлетворительное будущее!
Энергосберегающие решения: Забудьте о теплопотерях! Наши не только сохраняют тепло, но и дарят вашему жилищу новый качество энергоэффективности.
Сделайте свой домик теплым и изысканным!
Подробнее на [url=https://stroystandart-kirov.ru/]www.stroystandart-kirov.ru
[/url]
Не передавайте на произвол судьбы свой жилище на волю случая. Доверьтесь специалистам и создайте тепло вместе с нами!
Наша команда искусных мастеров завершена подать вам передовые системы, которые не только обеспечивают прочную охрану от заморозков, но и подарят вашему зданию современный вид.
Мы практикуем с современными веществами, подтверждая долгосрочный продолжительность использования и превосходные результаты. Утепление наружных поверхностей – это не только экономия на огреве, но и забота о экологии. Сберегательные инновации, какие мы используем, способствуют не только своему, но и поддержанию природных богатств.
Самое основное: [url=https://ppu-prof.ru/]Наружное утепление фасада цена[/url] у нас составляет всего от 1250 рублей за квадратный метр! Это бюджетное решение, которое превратит ваш резиденцию в настоящий тепловой локал с минимальными тратами.
Наши проекты – это не единственно изоляция, это постройка помещения, в где любой компонент отражает ваш собственный образ действия. Мы берем во внимание все твои требования, чтобы преобразить ваш дом еще еще более теплым и привлекательным.
Подробнее на [url=https://ppu-prof.ru/]http://www.ppu-prof.ru[/url]
Не откладывайте дела о своем корпусе на потом! Обращайтесь к мастерам, и мы сделаем ваш дом не только уютнее, но и стильнее. Заинтересовались? Подробнее о наших проектах вы можете узнать на веб-ресурсе. Добро пожаловать в обитель благополучия и уровня.
Online poker
Genuinely when someone doesn’t know afterward its up to
other people that they will help, so here it occurs.
RVVR is website dedicated to advancing physical and mental health through scientific research and proven interventions. Learn about our evidence-based health promotion programs. https://rvvr.us/
Colorado breaking news, sports, business, weather, entertainment. https://denver-news.us/
Find healthy, delicious recipes and meal plan ideas from our test kitchen cooks and nutrition experts at SweetApple. Learn how to make healthier food choices every day. https://sweetapple.site/
OCNews.us covers local news in Orange County, CA, California and national news, sports, things to do and the best places to eat, business and the Orange County housing market. https://ocnews.us/
Your source for Connecticut breaking news, UConn sports, business, entertainment, weather and traffic https://connecticutpost.us/
BioPharma Blog provides news and analysis for biotech and biopharmaceutical executives. We cover topics like clinical trials, drug discovery and development, pharma marketing, FDA approvals and regulations, and more. https://biopharmablog.us/
[url=https://gnesin-opera.ru]1хбет зеркало на сегодня[/url]– это популярная букмекерская контора, предоставляющая широкий выбор ставок на спорт и казино. Сайт обладает удобным интерфейсом, мобильной версией и приложением для удобства пользователей. 1xBet также известен разнообразными акциями и бонусами, делая игровой опыт более захватывающим.
East Bay News is the leading source of breaking news, local news, sports, entertainment, lifestyle and opinion for Contra Costa County, Alameda County, Oakland and beyond https://eastbaynews.us/
[url=https://myscoollife8.ru/]лучшие казино[/url]– это популярная букмекерская контора, предоставляющая широкий выбор ставок на спорт и казино. Сайт обладает удобным интерфейсом, мобильной версией и приложением для удобства пользователей. 1xBet также известен разнообразными акциями и бонусами, делая игровой опыт более захватывающим.
Greeley, Colorado News, Sports, Weather and Things to Do https://greeleynews.us/
Maryland Post: Your source for Maryland breaking news, sports, business, entertainment, weather and traffic https://marylandpost.us/
Baltimore Post: Your source for Baltimore breaking news, sports, business, entertainment, weather and traffic https://baltimorepost.us/
На сайте http://diplom-sale.ru возможно купить диплом о среднем специальном образовании [URL=http://diplom-sale.ru]http://diplom-sale.ru[/URL] с гарантией. Работаем со всеми образовательными учреждениями России.
The LB News is the local news source for Long Beach and the surrounding area providing breaking news, sports, business, entertainment, things to do, opinion, photos, videos and more https://lbnews.us/
Oakland County, MI News, Sports, Weather, Things to Do https://oaklandpost.us/
Ohio Reporter – Ohio News, Sports, Weather and Things to Do https://ohioreporter.us/
Recently, the industry has floated a proposal for enclosed smoking areas, but without giving details publicly. The Casino Association of New Jersey recently declined to provide details on its vision for smoking rooms. In a statement Thursday, the group said, “It is clear that more and more people realize that the bill, as drafted, will have a significant adverse effect on Atlantic City’s economy.” code: GODSOFWARVIP Below is a list of promotions currently being offered at Prism Casino. New post, Nina started a new topic: New Years Top 4 Winners! Prism Casino – Withdrawal remain unprocessed after timeframe Please understand that KYC is a very important and essential process, during which the casino makes sure that the money is sent to the rightful owner. As they don’t have the luxury of being able to physically see all of the players and check their identification and documents, this is the only way gambling establishments are able to complete the verification procedures. None of the serious and licensed casinos take KYC lightly and it might take a few working days to complete this thorough process.
https://directoryalbum.com/listings12632102/leovegas-casino-free-spins
Many online casino players are interested in sampling the last slot machine games, card games, table games, or other games for free. At 888casino NJ we offer many free casino games, including the latest releases. Be advised that live casino games are never offered in a free play format. Real Money Casino Gambling Once regulations for Ohio online casino sites are outlined by the law, we expect to see some of the best online casinos provide their services in the state. Residents of the state can look forward to accessing all of their favorite casino games through their mobile or desktop devices. Anyone above the legal age will be able to enjoy these services. This is a great idea, even if you’ve never heard of it before. This is the most popular option for free slots today. While many sites offer free casino games, very few have begun offering players the chance to download free slots. You will love it once you have tried it. This option might seem risky, so you won’t go to any site that doesn’t offer it.
These are our points of comparison to determine the best non GamStop casinos for UK players. Therefore, we can be sure that I have extensively tested all Bitcoin casinos for you. Only if these test points are met will we recommend one of the casinos for you. This is pretty self-explanatory. Some casinos offer only Bitcoin video slots, while others put an accent on table games like Bitcoin poker. Maybe you want to stake your cryptos in a Bitcoin live casino and measure your skill against other gamblers while a real croupier deals the cards. Although a Bitcoin casino with no deposit bonus may not make a very good impression at first glance, it might be the one that offers the perfect selection of games and policies for you. Launching in 2021, Bitstrike Casino has quickly become one of the best crypto and Bitcoin casinos for UK players. It was previously known as Bitslot casino but rebranded to its new name in 2023.
https://devinrnup863206.wizzardsblog.com/23853058/manual-article-review-is-required-for-this-article
“Every cash game I tested so far I tripled my stack in using the 6-pack profile.” Bitcoin is the future of online poker payments, due to its combination of security, privacy, and speed. The best bitcoin poker sites in the United States gaming market need to have several traits. First, the card site needs to support high limit bitcoin deposits and withdrawals. Second, an online poker room needs to make linking with your bitcoin wallet easy and instantaneous. The sites we suggest each have bitcoin tutorials with recommendations for bitcoin wallets while offering information on dozens of bitcoin exchanges. Whenever choosing a poker room to play on using credit card or PayPal to deposit, most players have to confirm their specific country is accepted for playing at the site. This is why we’re expanding a lot of the country guides as countries like India and Australia change the laws in gambling whenever they feel like. There are still many great poker sites that have better security, software and occasionally better games than crypto sites offer, so let’s hope more will add bitcoin deposits soon.
Hello, i think that i saw you visited my blog so i came to return the favor.I am attempting
to find things to enhance my web site!I suppose its ok to use a few of
your ideas!!
Way cool! Some extremely valid points! I appreciate you penning this
write-up and the rest of the site is really good.
You can see similar: dobry sklep and here dobry sklep
can i drink alcohol with zithromax
We are a group of volunteers and starting a new scheme in our community.
Your web site provided us with valuable info
to work on. You’ve done an impressive job and our whole community will be grateful to you.
LipoSlend is a liquid nutritional supplement that promotes healthy and steady weight loss. https://liposlendofficial.us/
Heya! I just wanted to ask if you ever have any problems with hackers?
My last blog (wordpress) was hacked and I ended up losing many months of
hard work due to no backup. Do you have any solutions to stop hackers?
I have read so many content concerning the blogger lovers however
this paragraph is truly a pleasant paragraph, keep it
up.
Incredible points. Great arguments. Keep up the amazing spirit.
zoloft maoi
furosemide in acute kidney injury
flagyl taste
high blood pressure medicine lisinopril
glucophage diarrhee
lasix eye
zithromax pneumonia
gabapentin for dogs dosage for pain
amoxicillin for pneumonia
drug gabapentin
cephalexin tablet
escitalopram 20mg tablets side effects
ciprofloxacin for cats
bactrim double strength
cephalexin 500 mg dosage
bactrim for kidney infection
does amoxicillin need to be refrigerated
para que sirve la cephalexin
is 300 mg of gabapentin, a low dose
escitalopram dosage amounts
Наша бригада квалифицированных мастеров подготовлена предложить вам инновационные системы, которые не только предоставят надежную защиту от холодных воздействий, но и преподнесут вашему собственности элегантный вид.
Мы функционируем с последовательными строительными материалами, заверяя долгосрочный время службы и отличные результаты. Утепление наружных стен – это не только экономия на подогреве, но и ухаживание о окружающей природе. Энергоспасающие методы, какие мы используем, способствуют не только твоему, но и сохранению природы.
Самое главное: [url=https://ppu-prof.ru/]Стоимость утепления фасада дома[/url] у нас стартует всего от 1250 рублей за кв. м.! Это доступное решение, которое переделает ваш хаус в реальный тепловой местечко с минимальными затратами.
Наши примеры – это не единственно изолирование, это постройка помещения, в где любой аспект символизирует ваш особенный модель. Мы примем все ваши желания, чтобы осуществить ваш дом еще более приятным и привлекательным.
Подробнее на [url=https://ppu-prof.ru/]http://www.ppu-prof.ru[/url]
Не откладывайте заботу о своем корпусе на потом! Обращайтесь к квалифицированным работникам, и мы сделаем ваш корпус не только более теплым, но и моднее. Заинтересовались? Подробнее о наших услугах вы можете узнать на официальном сайте. Добро пожаловать в мир благополучия и высоких стандартов.
what does citalopram look like
ddavp central di
is cozaar recalled
depakote generic name
cozaar indications
citalopram hydrobromide 20 mg high
ddavp used bed wetting
depakote dosages
is augmentin safe during pregnancy
ezetimibe combination therapy
diltiazem vs amlodipine
can you take diclofenac with tylenol
AUDI A3 (8L1) S3 quattro 2001 – 2003 165KW 224KM 1781ccm, BAM Audi A4 B5, rok produkcji: 1995-2001 Audi A4 B5, rok produkcji: 1995-2001 Jedynie zarejestrowani użytkownicy mogą komentować zawartość tej strony. Audi A4 B5, rok produkcji: 1995-2001 Audi 80 B4, rok produkcji: 1991-1995 kostka to kostka takie coś ze stykami sprzedawane pod nazwą handlową kostka stacyjki ale jak się nie znasz to oddaj do specjalisty. Na forum sporo razy poruszany temat wymiana kostki stacyjki Obudowa stacyjki (33) sprawdz czy nie zagial sie ktorys pin w kostce ewentualnie zimny lut puscilmniej prawdopodobne to kostka stacyjki.skontaktuj sie z mieto3 on postawi diagnoze a3-club.netforumshowthr…nikpost568987 a3-club.netforumshowthr…licznik&page2 Jedynie zarejestrowani użytkownicy mogą komentować zawartość tej strony.
https://pantip.com/profile/8006646#topics
2CD The Rolling Stones – GRRR. Rock UK. Rarytas. CD Używane Stan Jak Nowy Bez Jakichkolwiek Rysek. CD Wydanie Oryginalne Pełne (2012 r) 2CD Deluxe. Wydanie ABKC kołpaki 16 peugeot w Motoryzacja Jeszcze przed pierwszymi płatkami śniegu wielu z nas zadaje sobie to samo pytanie: Czy wybrać opony zimowe, czy może postawić na modele wielosezonowe? Odpowiedź może zależeć od wielu czynników, ale jedno jest pewne – bezpieczeństwo na drodze nie powinno być kompromisem. Ta aukcja dotyczy zestawu czterech (4) nowych, oryginalnie zapakowanych, najwyższej jakości KOŁPAKÓW w rozmiarze 16″. 2CD The Rolling Stones – GRRR. Rock UK. Rarytas. CD Używane Stan Jak Nowy Bez Jakichkolwiek Rysek. CD Wydanie Oryginalne Pełne (2012 r) 2CD Deluxe. Wydanie ABKC Jeszcze przed pierwszymi płatkami śniegu wielu z nas zadaje sobie to samo pytanie: Czy wybrać opony zimowe, czy może postawić na modele wielosezonowe? Odpowiedź może zależeć od wielu czynników, ale jedno jest pewne – bezpieczeństwo na drodze nie powinno być kompromisem.
does flomax cause kidney stones
effexor weight gain or loss
contrave 4 pills a day
flexeril image
Hi! Do you know if they make any plugins to protect against
hackers? I’m kinda paranoid about losing everything I’ve worked hard on. Any suggestions?